Abstract
The opioid overdose crisis is a public health emergency in Canada (Public Health Agency of Canada, 2022). It is estimated that there have been 30,843 opioid-related deaths in Canada between January 2016 and March 2022, and most of those deaths (85%) have been linked to the unregulated drug market containing fentanyl (Public Health Agency of Canada, 2022). Although there are regional differences with respect to the illicit drug supply, the opioid poisoning crisis is occurring across Canada (Morrison et al., 2017). Fentanyl is a synthetic opioid that is highly potent and is often cut into other illicit drugs (Han et al., 2019). Fentanyl, along with other substances, increases the risk of opioid poisoning for people who use drugs (PWUD; Kolla et al., 2022; McDonald et al., 2020; Tyndall, 2020). For example, McDonald et al. (2020) found that 43% of heroin purchased illicitly contained fentanyl in samples taken from the Greater Toronto area in 2019–2020. In addition to the risk of injecting unregulated drugs, injection drug use can increase the risk for infectious conditions, including general skin infections, HIV/AIDS, and hepatitis C (HCV; Bonn et al., 2020; Shayan et al., 2021).
Harm Reduction
To address the risk associated with injection drug use, harm reduction initiatives emerged for PWUD. Harm reduction programs aim to reduce overdose risk, the transmission of communicable diseases, and other unsafe drug practices (Tzemis et al., 2013). These services are not based on traditional abstinence models (e.g., detoxification, inpatient rehabilitation, etc.), but on offering support to PWUD through increasing the safety of their drug use (Tyndall, 2020). Such programs are beneficial to individuals who either are not successful or are not interested in abstinence-based programs (Brar et al., 2019). Harm reduction initiatives include clean needle supply, opioid-assisted treatment (OAT; such as methadone or buprenorphine maintenance programs), drug testing, naloxone overdose distribution kits, supervised injection sites, and more recently, safer supply programs (SSPs; Ivsins et al., 2020; Mrazovac et al., 2020).
Safer Supply Programs
The presence of powerful opioids such as fentanyl in the drug market has rendered traditional OAT as insufficient to address the opioid crisis, partly due to increased tolerance to opioids in PWUD (Bonn et al., 2021). SSPs are settings where individuals are prescribed pharmaceutical drugs (e.g., hydromorphone, diacetylmorphine) that can be safely consumed as a substitution for unregulated street drugs (Ivsins et al., 2020). In addition to regulated drugs, individuals are provided with clean equipment, and access to other resources and social supports (Pauly et al., 2020). Canada’s first SSP opened in 2016 in Ontario (Gomes et al., 2022). There are currently 28 SSPs operating across Canada, some funded by Health Canada’s Substance Use and Addiction Program (SUAP), although there are also SSPs operating outside of this funding (Glegg et al., 2022; Government of Canada, 2023). Of the SUAP funded SSPs, the majority are located in Ontario and British Columbia (15 and 11, respectively), with the other two sites being located in the provinces of Quebec and New Brunswick (Government of Canada, 2023). Glegg et al. (2022) identified, in an environmental scan, 103 SSPs operating across Canada.
Research shows that SSPs are a cost-effective intervention that improve the health and social well-being of individuals in the programs (Brar et al., 2019; Gomes et al., 2022; Ivsins et al., 2020, 2021). In addition, as injections are usually supervised, overdose mortality is reduced, which is critical to addressing the opioid poisoning crisis (Levengood et al., 2021). Lastly, SSPs have been shown to lower the crime rates in the areas where they are located (Levengood et al., 2021; Marshall et al., 2011) as PWUD are less likely to participate in illegal activities in order to access drugs (Bonn et al., 2020). Despite the emerging evidence regarding the positive impact of SSPs, these services remain somewhat controversial. The concerns generally stem from the belief that SSPs, like OAT, provide ‘replacement’ drugs rather than abstinence from substances, which is often viewed among the general population as the desirable option (Steel & Tekin, 2021). Abstinence-based models, however, are not appropriate for all individuals (Brar et al., 2019). In a review by Brorson et al. (2013), dropout rates in traditional abstinence-based treatments ranged from 22%–43% for detoxification programs, 23%–50% for outpatient programs, and 17%–57% for inpatient programs. Furthermore, OATs (e.g., methadone maintenance programs) had dropout rates that ranged from 32%–68% (Brorson et al., 2013). These statistics highlight the need for alternative models that are not based on abstinence, and that reduce access barriers.
Attitudes Towards SSPs
It is important to consider the public’s attitudes surrounding harm reduction, as public support has a direct impact on policymaking, funding, as well as the implementation and operational practices of these programs (Karamouzian et al., 2023; Wild et al., 2021). Public support for harm reduction approaches in the Canadian population is polarized, with 64% of the general population approving these initiatives overall (Wild et al., 2021). In the same study, public support for supervised injection sites was endorsed by 55% of the sample, and low-barrier OAT (i.e., methadone, buprenorphine) was supported by 49% of Canadians. Support for SSPs has been recently evaluated in the Canadian Prairies, where SSPs were supported by 56.3%–63.5% of the sample, depending on the province (Morris et al., 2023). However, such an evaluation is also necessary elsewhere in Canada, as attitudes are likely to differ based on geographical location.
The ‘not in my backyard’ (NIMBY) phenomenon represents individuals who may approve of harm reduction initiatives in a broader sense, but not when the initiatives are specific to their own communities. Socia et al. (2021) demonstrated this phenomenon in a study where participants were found to be less supportive of safe injection facilities within their own communities compared to elsewhere in the United States. To a lesser effect, the NIMBY effect was demonstrated in Canada with respect to clean needle distribution in British Columbia, where 72% of the public was found to be supportive of clean needle distribution generally, but 65% agreed if the program would take place in their own communities (Tzemis et al., 2013). Additionally, in a study by Javadi et al. (2022), the authors found that only 28% of substance use treatment professionals reported being comfortable with a safer consumption site opening within their own communities. This NIMBY effect has been posited to stem from the belief that these initiatives will decrease property values, and increase crime rates and public drug use, although the opposite impact has generally been shown (Bonn et al., 2020; Kolla et al., 2017; Levengood et al., 2021). As such, the current study examined public support for SSPs overall and within the participant’s community, to examine if the NIMBY effect would emerge. A second goal of the study was to examine the factors that affect attitudes towards SSPs as this may help to develop targeted public awareness campaigns.
Impact of Demographic Factors on Harm Reduction Attitudes
Tzemis et al. (2013) completed a study on attitudes towards general harm reduction initiatives (e.g., programs that aim to promote safer drug use) in British Columbia, Canada, and found that males were 26% less likely to support harm reduction initiatives when compared to females. Age and educational status were also shown to be significant predictors of positive attitudes towards harm reduction, with younger individuals, and those with higher levels of education being more supportive (Tzemis et al., 2013). Higher educational status has been shown to be significantly associated with more positive attitudes towards harm reduction in additional studies (Morris et al., 2023; Mrazovac et al., 2020; Wild et al., 2021).
Impact of Personality on Harm Reduction Attitudes
One factor which may affect attitudes toward substance use interventions is personality. The Five-Factor Model posits that individuals vary on five personality dimensions, including Openness to Experience (e.g., creative, curious), Conscientiousness (e.g., organized, ambitious), Extraversion (e.g., talkative, passionate), Agreeableness (e.g., trusting, generous), and Neuroticism (e.g., temperamental, emotional; Costa & McCrae, 1992). Lower Extraversion and higher Openness to Experience have been found to predict more positive attitudes towards drug decriminalization (MacQuarrie & Brunelle, 2022). No research has examined if these personality factors may predict attitudes towards harm reduction, specifically SSPs. However, several studies have examined the associations between personality and drug use (Benotsch et al., 2013; Terracciano et al., 2008; Turiano et al., 2012). Overall, individuals who score higher in Neuroticism and Openness to Experience, and lower in Conscientiousness, have been found to exhibit increased substance use (Benotsch et al., 2013; Turiano et al., 2012).
Impact of Stigma on Harm Reduction Attitudes
In addition to personality, attitudes towards harm reduction may also be influenced by stigma, which includes negative beliefs towards a group (i.e., stereotyping) or behavioural actions (i.e., discrimination) towards an individual or group (Link & Phelan, 2001). Additionally, stigma can be categorized into public stigma (the views/discrimination of the public towards a population) and self-stigma (one’s stigmatized views towards themselves due to a diagnosis/situation; Yuan et al., 2018). Increased stigma towards PWUD has been shown to negatively affect attitudes towards harm reduction services (Reynolds et al., 2022; Wild et al., 2021). The war on drugs and the resulting criminalization of PWUD has greatly contributed to the stigma surrounding PWUD, as the public begins to place the blame on the individual for using drugs and believes that criminalization is the most effective way to address substance use (Tyndall & Dodd, 2020). Reynolds et al. (2022) assessed stigma levels by presenting Canadian university students with vignettes depicting fictitious opioid users seeking various harm reduction services (i.e., no harm reduction services, OAT, for safer consumption sites). Results showed that participants held less stigma towards vignette characters who were using OATs, compared to the characters not using any harm reduction services. Researchers also noted a trend of higher stigma levels towards vignette characters using safer consumption sites when compared to OATs.
Stigma, Personality, and Attitudes Towards Harm Reduction
There is a lack of research on public attitudes towards SSPs, and, to our knowledge, no study has examined the role of personality and stigma on attitudes towards SSPs. However, Wild et al. (2021) found that stigmatized attitudes towards PWUD negatively impacted public support towards harm reduction services. Stigma levels towards PWUD may influence attitudes towards harm reduction indirectly because they impact personality factors. Brown (2023) evaluated self-stigma (an individual’s internalization of public stigma) and found that higher neuroticism and lower conscientiousness accounted for a large proportion of variance in a substance user’s negative attitudes towards themselves, showing a relationship between stigma and personality. In addition, Yuan et al. (2018) found that high agreeableness and openness to experience were associated with reduced stigma towards people with mental disorders. These findings suggest that personality is associated with stigma towards substance users. Hence, the mediating role of personality in the relationship between stigma towards PWUD and attitudes towards SSPs will be examined in the current study.
Present Study
The purpose of the current study was to (1) assess current attitudes towards SSPs in New Brunswick, Canada, (2) determine factors (i.e., demographic factors, personality, stigma) that predict attitudes towards these services and (3) examine whether personality mediates the relationship between the stigmatization of PWUD and attitudes towards SSPs. Based on previous research, it was hypothesized that a younger age would be predictive of supportive attitudes towards SSPs (Tzemis et al., 2013). Next, it was hypothesized that those who identify as female would be more supportive of SSPs than those who identify as male, and that higher educational status would be associated with more positive attitudes towards SSPs (Mrazovac et al., 2020; Tzemis et al., 2013; Wild et al., 2021). Furthermore, it was expected that Openness to Experience would be associated with more positive attitudes towards SSPs (Benotsch et al., 2013; MacQuarrie & Brunelle, 2022; Turiano et al., 2012), and that personality would mediate the relationship between stigma towards PWUD and attitudes towards SSPs (Brown, 2023; Wild et al., 2021; Yuan et al., 2018).
Method
Participants
Demographic Statistics.
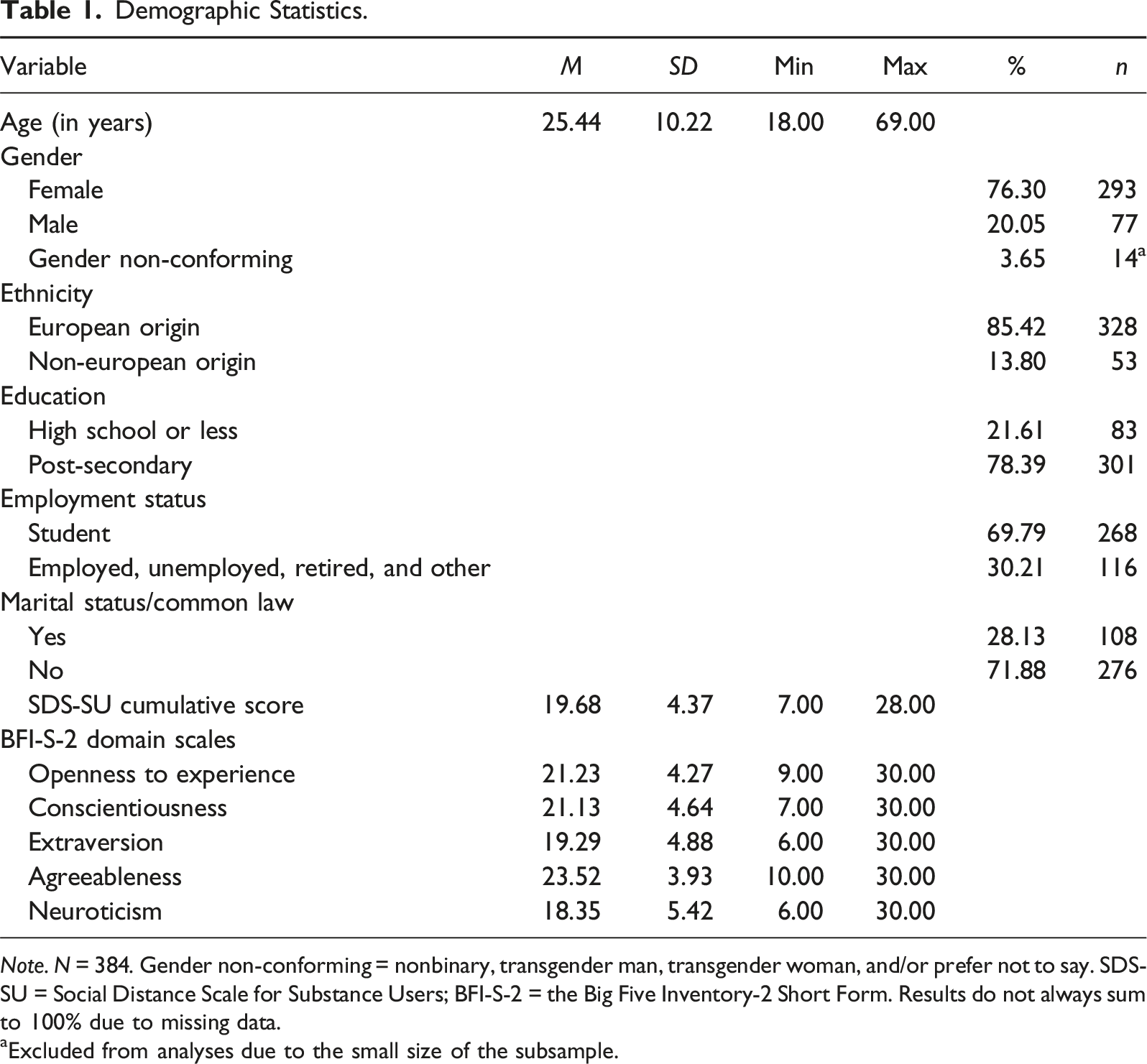
aExcluded from analyses due to the small size of the subsample.
Measures
Demographics
An internally generated demographics questionnaire assessed participants’ age, gender identity, ethnicity, occupation, education, and marital status.
The Big Five Inventory - Short Form
To assess personality, the Big Five Inventory - Short Form (BFI-2-S; Soto & John, 2017) was used. The BFI-2-S is one of the most established measures of the five-factor personality model and has been shown to have excellent reliability and validity (Soto & John, 2017). The BFI-2-S has five subscales, measuring Openness to Experience, Conscientiousness, Extraversion, Agreeableness, and Neuroticism. Participants rate the applicability of 30 statements to themselves, on a five-point scale, ranging from disagree strongly to agree strongly. Following the reverse scoring of select items, scores were summed for each subscale, with higher scores indicating increased levels of that trait. Internal consistencies for the subscales ranged from α = .70–.83.
Social Distance Scale for Substance Users
The Social Distance Scale for Substance Users (SDS-SU; Brown, 2011) was used to measure stigma levels towards PWUD. The SDS-SU has been shown to have good psychometric properties and has been used in previous studies to measure stigma towards people who use substances (Brown, 2015; Wild et al., 2021). The SDS-SU includes seven questions (e.g., “how would you feel about renting a room in your home to someone with a substance use problem”) that are rated on a four-point scale ranging from definitely willing to definitely unwilling. Questions were modified slightly to suit the needs of the study, and to adapt to more appropriate language (e.g., the statement “How would you feel about introducing someone with a substance use problem to a young woman you are friendly with?” was changed to “how would you feel about introducing a person with a substance use problem to your friends?”). Participants' scores were summed for all questions, with higher scores indicating increased stigma levels. The internal consistency for the SDS-SU was good (α = .81).
Internally Generated Questions - SSP Attitudes
Participants were first provided with a general definition of SSPs, which stated “Safer supply programs allow individuals to receive a prescription for a pharmaceutical drug that can be used as a replacement to drugs available in the illicit market (street drugs). Some community settings also provide access to healthcare, clean needles, a supervised place to use the prescribed drugs, and access to other supports.” Attitudes towards SSPs were measured on a five-point scale ranging from strongly disagree to strongly agree. Two statements were included: “In general, I support the use of safer supply programs as a form of harm reduction” and “I support the use of safer supply programs as a form of harm reduction within my own community.” Higher scores were indicative of increased support for SSPs.
Procedure
Undergraduate participants from the university where the study took place accessed the link for the Qualtrics survey through the university’s research system, SONA. Participants from the general public accessed the link for the online survey through social media posts. The survey took approximately 15 minutes to complete and was approved by the institution’s research ethics board prior to being administered.
Results
Preliminary Analyses
Prior to data analyses, data were cleaned, with responses that were completed in a short amount of time (i.e., under 2 minutes), exhibited unusual response patterns (i.e., robot activity or automatically clicking random responses), or responses with more than 20% missing data being removed (
Public Attitudes
Public attitudes towards SSPs were considered supportive if participants responded with “strongly agree” or “agree” to the statement “In general, I support the use of safer supply programs as a form of harm reduction.” When asked about their support for SSPs in general, 82.3% (
Predictors of Attitudes Towards SSPs
Hierarchical Regression for Attitudes Towards SSPs.

*
The overall model was significant
Personality as a Mediator
As Openness to Experience and stigma were both significant predictors of attitudes towards SSPs, a mediation analysis was performed to examine if the trait Openness to Experience would emerge as a mediating variable between stigma towards PWUD and attitudes towards SSPs.
A 5000-sample bootstrapping mediation analysis using the PROCESS macro, version 4.2 (Hayes, 2022) was conducted to examine the relationship between stigma levels and attitudes towards SSPs and the indirect effect of Openness to Experience. A significant direct or indirect effect is found when the 95% confidence interval does not cross zero. A direct relationship between stigma towards PWUD and attitudes towards SSPs was found, 95% CI [−.0865, −.0402], indicating that those scoring higher on stigma are more likely to have negative attitudes towards SSPs. The indirect relationship through Openness to Experience also emerged 95% CI [−.0089, −.0005], indicating that Openness to Experience partially mediated the relationship between stigma towards PWUD and attitudes towards SSPs.
Discussion
The current study assessed attitudes towards SSPs as well as the factors that influence these attitudes, specifically the impact of demographics, personality, and stigma in a sample of Atlantic Canadians. In the current study, 82.3% of the sample was supportive of SSPs overall, which represents an elevated level of agreement within this sample as compared to other studies that examined attitudes towards harm reduction generally (64%; Wild et al., 2021) or SSPs specifically (56.3%–63.5%; Morris et al., 2023). These findings may be explained by the nature of the current sample. The only study examining attitudes towards SSPs (Morris et al., 2023) was conducted in the Canadian Prairies, a geographic area that has recently experienced a policy shift to an abstinence-based model of care, which has affected the implementation of harm reduction initiatives in this geographical area (Brooks et al., 2022) and may have impacted attitudes towards SSPs. Furthermore, research has shown that females, those of a younger age, and individuals with increased levels of education are more likely to support harm reduction initiatives (Cruz et al., 2007; Morris et al., 2023; Mrazovac et al., 2020; Tzemis et al., 2013; Wild et al., 2021). The current sample mostly identified as female (76.3%), younger (mean age of 25.4 years), and the majority (78.4%) of participants reported having post-secondary education, which may explain why the current sample was overall in favour of SSPs.
Within the current study, 79.7% of the sample indicated that they would be supportive of SSPs being located within their own communities. Approval for SSPs located within one’s own community was statistically lower than overall support for these programs, which is in line with previous research (Javadi et al., 2022; Socia et al., 2021; Tzemis et al., 2013). However, the difference was modest. This might be suggestive that the NIMBY phenomenon, where individuals are less likely to support harm reduction initiatives within their own communities, is attenuating as the Canadian population becomes more aware of the opioid crisis (Morris et al., 2023) and that the population witnesses the positive impact that harm reduction services are exerting in their communities. In a study interviewing community and business members in Ontario, Canada (Kolla et al., 2017), it was found that it was essential that residents perceive that supervised consumption services have community benefits (e.g., reduced public drug use and drug-related litter) that go beyond benefits for PWUD (i.e., reduced opioid poisonings) in order to have more positive attitudes towards these services.
Results from the hierarchical linear regression showed that taken together, identifying as female, of European origin, being younger, more open to experience and having less stigmatizing attitudes towards PWUD accounted for 17.1% of the variance in attitudes towards SSPs. This is a relatively small proportion of variance, and other factors are likely to also contribute to attitudes (e.g., religious and political affiliations; Adams et al., 2018; Barry et al., 2014), however, these variables remain important to consider. The demographic predictors of more positive attitudes towards SSPs are in line with previous research, except for education levels, which did not emerge as a significant predictor of attitudes. However, this finding may be due to a lack of overall variability in educational levels in the current sample. A novel finding of the current study is the emergence of the personality trait Openness to Experience as a predictor of more positive attitudes towards SSPs. Although no research has examined personality as a predictor of attitudes towards SSPs, a recent study by MacQuarrie and Brunelle (2022) found that Openness to Experience significantly predicted more supportive attitudes towards drug decriminalization. Openness to Experience has also been linked with individual drug use and so the current results may reflect a higher tolerance for drug use in general, translating into increased comfort with harm reduction services for PWUD (Benotsch et al., 2013; Turiano et al., 2012).
Decreased stigma levels towards PWUD were also a significant predictor of more positive attitudes towards SSPs. Increased stigma has previously been associated with negative attitudes towards harm reduction (Reynolds et al., 2022; Wild et al., 2021). Stigma towards PWUD and harm reduction initiatives may be fueled by drug policies that focus on criminalization rather than rehabilitation, according to a recent Canadian study conducted with PWUD (Scher et al., 2023). As a consequence, the public may be more likely to support treatment initiatives that focus on abstinence rather than reducing the harms associated with drug use (McGinty et al., 2018). Although McGinty et al. (2018) suggested that stigma towards mental illness and substance use could be targeted by using communication strategies that are based on PWUD’s personal experiences and also highlight structural barriers (e.g., lack of treatment accessibility), destigmatization may only truly occur in the context of drug decriminalization policies.
Results from the mediation analyses showed a direct relationship between stigma and attitudes towards SSPs. The personality trait Openness to Experience was also a significant mediator in this relationship, meaning that stigma towards PWUD is related to more negative attitudes towards SSPs, in part because individuals with higher stigmatizing beliefs are less Open to Experience. These findings suggest that it may be important to tailor public health messaging to psychological factors such as personality. One size fits all public health campaigns may not be as effective as when messaging is directly targeted to certain subgroups of individuals (Alsan et al., 2021). As such, the findings of the current study suggest that individuals who share certain characteristics (e.g., middle aged, less educated, from ethnic minorities, etc.) may benefit from public messaging regarding substance users and harm reduction initiatives that is directly addressing their concerns. Future research should examine the specific reasons why certain individuals are not supportive of harm reduction initiatives in order to target these specifically.
Limitations
The main limitations of the current study include the composition of the sample, which is comprised primarily of individuals identifying as female, of a younger age, and educated. Although online surveys generally favour participation from those who identify as female (Ryan et al., 2019), the age and educational profile of the sample may be due to approximately half of the participants having been recruited from an undergraduate university setting. Due to these sample characteristics, the current study should be replicated in a more representative sample of the general Canadian population. Lastly, when measuring attitudes through a self-report measure, participants may be more likely to report positive attitudes to adhere to what they expect the desired outcome to be (Arnold & Feldman, 1981), which may have contributed to more positive attitudes towards SSPs.
Conclusion
The opioid overdose crisis is a public health emergency in Canada, and SSPs are part of the solution to address this crisis. Although the majority of the variables used in the current study to predict attitudes towards SSPs cannot be modified (e.g., demographics), stigma can be targeted in an attempt to increase positive attitudes towards SSPs, which thereby is likely to increase support for the policies surrounding these programs (McGinty et al., 2018). Public awareness campaigns have been used in the past to reduce stigma towards people with mental illness (Collins et al., 2019). Such approaches are essential in order to facilitate the expansion of SSPs in Canada and address the growing opioid epidemic.
