Abstract
Introduction
Endometrial carcinoma (EC) is one of the most prevalent gynecologic malignancies globally, accounting for approximately 417,367 new cases and 97,370 deaths globally in 2020. 1 Notably, 75–80% of cases are diagnosed at early stages. 2 Although 85% of early-stage patients achieve favorable outcomes, with 5-year survival rates exceeding 90% following surgical intervention, a clinically significant proportion (7–15%) experience disease recurrence within 3–5 years, resulting in a substantially worse prognosis.2,3 Traditional recurrence risk assessment relies on clinicopathological factors, including tumor grade, depth of myometrial invasion, and lymphovascular space involvement, which are used to stratify patients into risk groups to guide postoperative management.4–6 Recently, the development of The Cancer Genome Atlas (TCGA) classification system has provided a supplementary molecular framework for patient stratification and treatment guidance. 7 This classification identifies four molecular subtypes with distinct clinical behaviors: POLE-ultramutated, microsatellite instability (MSI), copy-number low (CN-L), and copy-number high (CN-H). While the POLE-ultramutated and CN-H subtypes demonstrate clear prognostic extremes, the MSI and CN-L subgroups, which comprise more than 60% of cases, show overlapping survival outcomes (5-year recurrence-free survival: 72% vs. 74%), 8 highlighting the need for additional biomarkers to further optimize risk stratification within these intermediate molecular categories.
Autophagy, an evolutionarily conserved lysosomal degradation pathway, serves as a critical quality control mechanism that maintains cellular homeostasis through the regulated turnover of damaged organelles and protein aggregates. 9 In cancer biology, autophagy plays context-dependent roles: during tumor initiation, it functions as a tumor-suppressive mechanism by preventing genomic instability through the clearance of damaged cellular components; whereas in established malignancies, autophagy supports tumor cell survival by mitigating metabolic stress, hypoxia, and therapeutic challenges. 10 In EC, the AKT‒nuclear factor (NF)κB signaling axis has been shown to activate cancer-promoting autophagy, which facilitates EC cell growth and metastatic dissemination. 11 Furthermore, the inhibition of autophagy potentiates the antitumor effects of β-catenin pathway inhibitors in EC models, suggesting that autophagy mediates therapeutic resistance in this malignancy. 12 Importantly, emerging evidence indicates that autophagy activity varies significantly across molecular subtypes of cancer. In breast cancer, for example, the autophagy regulator BECN1 has subtype-specific expression patterns, with the lowest levels observed in aggressive human epidermal growth factor receptor 2 (HER2)-enriched and basal-like tumors, where it is correlated with TP53 mutations and advanced disease. 13 These observations suggest that systematic evaluation of autophagy-related molecular signatures could yield clinically relevant biomarkers.
By systematically evaluating autophagy-related genes within the TCGA framework and validating findings using clinical specimens and information from our institution, this study identified potential prognostic biomarkers that enhance risk stratification, particularly for distinguishing MSI and CN-L subtypes with overlapping recurrence risks. This integrated approach not only augments the clinical utility of the TCGA classification but also provides novel insights for personalized postoperative management.
Materials and methods
Data acquisition and processing
RNA sequencing profiles and clinical information for early-stage EC (International Federation of Gynecology and Obstetrics (FIGO) stages I and II) samples were obtained from the TCGA database. Molecular classification data for early-stage EC were retrieved from cBioPortal for Cancer Genomics. 14 A total of 222 autophagy-related genes (ARGs) were obtained from the Human Autophagy Database (HADb, https://www.autophagy.lu/v1/index.html), and their associations with EC patient prognosis were analyzed. Samples meeting the following criteria were used for subsequent analysis: (a) complete survival information; and (b) follow-up time > 90 days. To ensure analytical reliability, transcripts with transcripts per million(TPM) values of 0 in more than 50% of the samples were excluded, resulting in 366 retained for subsequent analysis (Supplemental Table 1).
Identification of survival-related autophagy genes
Principal component analysis was used to visualize the expression patterns of early EC and adjacent normal tissues. Univariate Cox regression analysis and Kaplan–Meier analysis were performed to assess the associations of all ARGs with overall survival (OS) and disease-free survival (DFS) in patients with early-stage EC. Multivariate Cox regression analysis was subsequently conducted to identify independent risk factors among the messenger RNAs (mRNAs) significantly associated with outcomes via univariate analysis.
Analyzing the relationship between ARGs and TCGA molecular classification
To understand the basic characteristics of molecular typing in early-stage EC patients, survival outcomes were assessed across all four TCGA molecular subtypes (POLE-ultramutated, MSI, CN-L, and CN-H) in early-stage EC patients using the Kaplan–Meier analysis. We subsequently conducted focused Kaplan–Meier survival analyses to compare recurrence-free survival and OS between patients with high PEA15-expressing tumors and those with low PEA15-expressing tumors exclusively within the MSI and CN-L patient subgroups.
Tissue samples
Ninety-nine early-stage EC samples from patients who did not receive chemotherapy or radiotherapy were collected from surgical resections for immunohistochemistry analysis. These samples were obtained from Union Hospital, Tongji Medical College, Huazhong University of Science and Technology, and written informed consent was obtained prior to surgery between January 2011 and December 2017. All procedures involving clinical samples and patient information were approved by the Medical Ethics Committee, Union Hospital, Tongji Medical College, Huazhong University of Science and Technology. Patients were followed until November 2022. OS was defined as the time from surgery to the last follow-up or death, whereas DFS was measured from surgery to the last follow-up, death, or cancer recurrence confirmed by radiographic and pathological evidence. A tissue microarray from each tumor was constructed by Wuhan Powerful Biology for standardized immunohistochemical analysis.
Immunohistochemistry
A standard immunohistochemistry (IHC) protocol was used to detect the protein level of PEA15. Briefly, formalin-fixed, paraffin-embedded EC tissues were deparaffinized and hydrated by sequential washes with xylene, anhydrous ethanol, 95% ethanol, 75% ethanol, 50% ethanol, and phosphate-buffered saline (PBS). After heat-induced antigen retrieval, a hydrogen peroxide solution was used to inactivate endogenous peroxidases. Non-specific binding sites were subsequently blocked with 10% goat serum. The sections were incubated overnight with anti-PEA15 antibody (1:200 dilution, Proteintech, 21446-1-AP, China) at 4°C. The sections were subsequently incubated with enhanced enzyme-labeled goat anti-rabbit IgG polymer at 37°C for 20 min, followed by 3,3′-diaminobenzidine staining and counterstaining with hematoxylin. The IHC results were scored according to the following formula: staining intensity (none = 0, weak = 1, moderate = 2, strong = 3) and staining area (less than 5% = 0, between 5% and 25% = 1, between 25% and 50% = 2, between 50% and 75%=3, and more than 75% = 4). The final staining score was calculated by multiplying the staining intensity and area scores, with positivity graded as follows: 0 (negative, −), 1–4 (weakly positive, +), 5–8 (positive, ++), and 9–12 (strongly positive, +++).
Statistical analysis
All the statistical analyses were performed using the R environment (version 3.6.3), GraphPad Prism (version 8.3.0), and SPSS (version 23). Survival-associated genes were identified through univariate and multivariate Cox regression analyses. Kaplan–Meier survival curves and log-rank tests were employed for survival analysis, whereas the chi-square test was used to assess correlations between IHC scores and tumor recurrence, as well as between PEA15 expression and clinicopathologic features. A
Results
Screening of ARGs associated with prognosis
The transcriptome of the TCGA-Uterine Corpus Endometrial Carcinoma (UCEC) cohort, which included 366 early-stage EC samples and 14 adjacent endometrial tissue samples, was acquired from the TCGA project (Supplemental Table 1). Principal component analysis revealed distinct expression patterns of ARGs between early-stage EC tissues and adjacent non-cancerous endometrium. As shown in Supplemental Figure 1a, the ARG expression profiles of all early-stage EC samples clearly separated from those of adjacent endometrial tissues, indicating significant differences in autophagy-related transcriptional activity between cancerous and non-cancerous tissues. This separation was further validated in a subset of 14 paired early-stage EC and adjacent endometrial tissues (Supplemental Figure 1b), where the paired samples exhibited consistent clustering patterns, reinforcing the robustness of the observed differences. These findings suggest that the expression of ARGs is systematically altered in early-stage EC, highlighting their potential role in tumor development and progression.
To identify ARGs associated with prognosis, univariate Cox regression analysis was performed for OS and DFS. The analysis revealed that 28 ARGs, including 26 high-risk genes and 2 low-risk genes, were significantly associated with OS (Figure 1(a)). Similarly, 20 ARGs, comprising 18 high-risk genes and 2 low-risk genes, were linked to DFS (Figure 1(b)). Among these, nine ARGs—

Identification of ARGs associated with survival. (a) Forest plot illustrating ARGs associated with OS based on univariate Cox regression analysis. Red denotes genes with a HR > 1, whereas green represents genes with an HR < 1. (b) Forest plot illustrating ARGs associated with DFS based on univariate Cox regression analysis. Red denotes genes with a HR > 1, whereas green represents genes with an HR < 1. (c) Kaplan–Meier curves showing OS for groups with high and low expression levels of the respective genes. (d) Kaplan–Meier curves showing DFS for groups with high and low expression levels of the respective genes.
Correlation analysis revealed significant co-expression among five genes—
Combined application of molecular classification of ARGs and TCGA molecular classification
The Kaplan–Meier survival analysis revealed significant differences in OS (Figure 2(a)) and DFS (Figure 2(b)) among the four subtypes based on TCGA molecular classification of early-stage EC patients (all
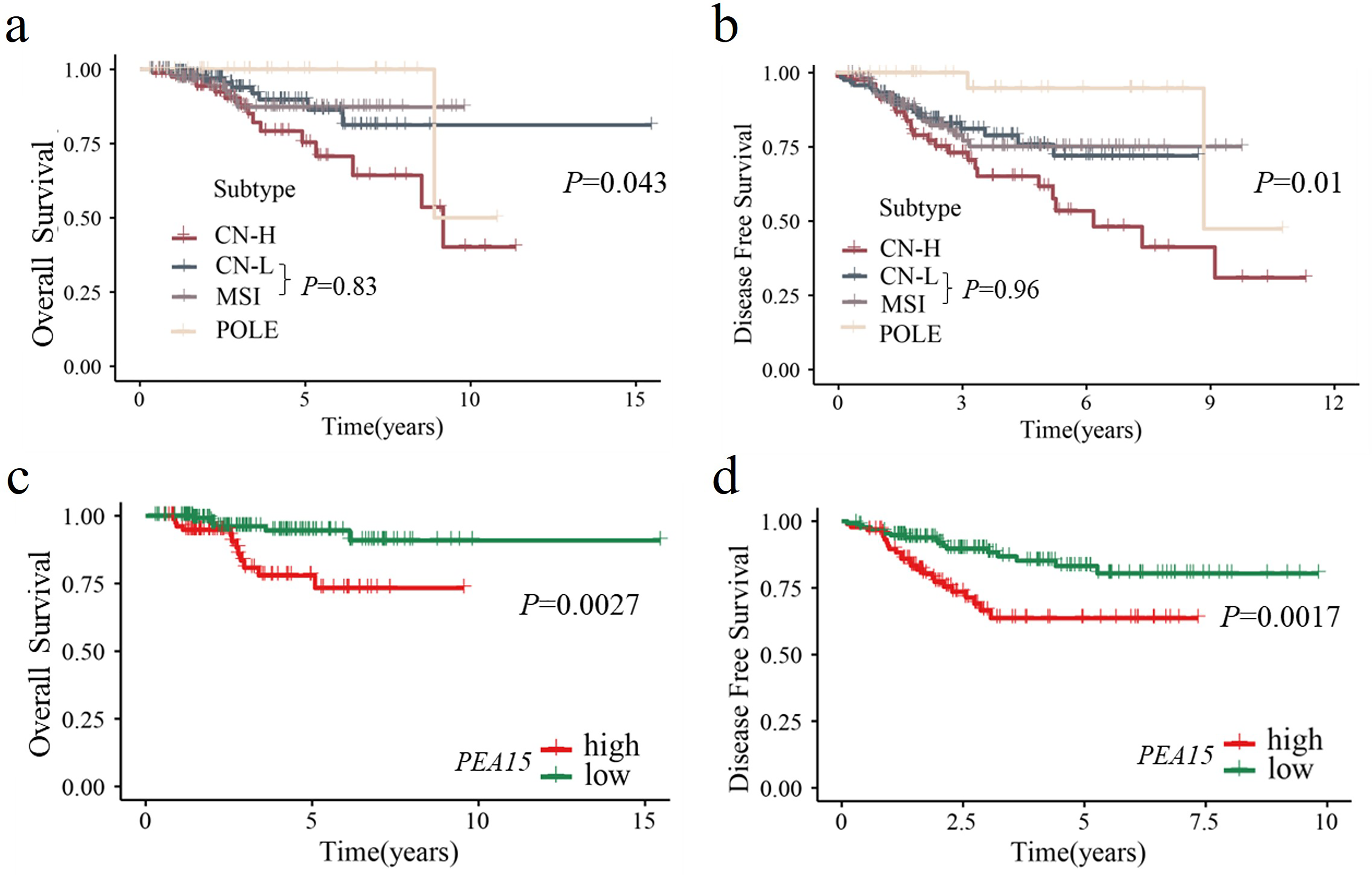
Kaplan–Meier curves of TCGA molecular classification and its correlation with PEA15. (a) Kaplan-Meier curves showing OS for early-stage endometrial cancer patients stratified by TCGA molecular classification: POLE, MSI, CN-L, and CN-H. (b) Kaplan–Meier curves showing the DFS of early-stage endometrial cancer patients stratified by TCGA molecular classification. (c) Kaplan–Meier curves showing OS for groups with high and low expression levels of
Expression of PEA15 protein and prognosis in early-stage EC
To evaluate the protein expression of PEA15 in early-stage EC, IHC was performed on 99 early-stage EC samples (Supplemental Figure 3). PEA15 exhibited a distinct cell type-specific distribution, with prominent cytoplasmic expression observed in tumor cells and vascular smooth muscle cells. In contrast, other stromal components showed either no detectable expression or only faint, scattered positive expression. Among the tumor cells, PEA15 staining intensity varied across the cohort, ranging from negative (−) to strong (+++). For subsequent analyses, cases were stratified into two groups: low PEA15 expression (negative (−) or weak positive ( + )) and high PEA15 expression (positive (++) or strong positive (+++)).
The associations between PEA15 expression (high vs. low) and clinicopathological features—including age (< 60 years vs. ≥ 60 years), FIGO stage (IA vs. IB vs. II), histological grade (G1 vs. G2 vs. G3), depth of myometrial invasion (inner 1/2 vs. outer 1/2), pathological type (endometrioid adenocarcinoma vs. non-endometrioid adenocarcinoma), and lymphovascular space invasion (LVSI) status (positive vs. negative)—were further examined using the chi-square test. As summarized in Table 1, no significant correlations were observed between PEA15 expression and any of the clinicopathological parameters (all
Correlations between PEA15 expression and clinicopathological features in early-stage EC patients.

FIGO: International Federation of Gynecology and Obstetrics; LVSI: lympho-vascular space invasion.
Kaplan–Meier survival analysis revealed that patients with high PEA15 expression had significantly shorter OS (

Kaplan–Meier survival analysis of PEA15 expression in early-stage EC patients by IHC. (a) Kaplan–Meier curves showing OS for groups with high and low PEA15 expression levels in patients with early-stage EC at our institution. (b) Kaplan–Meier curves showing DFS for groups with high and low PEA15 expression levels in patients with early-stage EC at our institution.
Univariate and multivariate cox regression analyses of DFS in patients with stage I endometrioid adenocarcinoma (n = 94).

CI: confidence interval; FIGO: International Federation of Gynecology and Obstetrics; HR: hazard ratio; LVSI: lympho-vascular space invasion.
Discussion
The molecular classification of EC proposed by the TCGA has significantly advanced our understanding of the disease by categorizing EC into four subtypes:
The TCGA molecular classification has emerged as a cornerstone in EC research, providing a framework for understanding tumor heterogeneity and guiding personalized treatment strategies. Recent studies have explored new molecular markers to complement TCGA classification. For example, Kommoss et al. identified L1 cell adhesion molecule (L1CAM) protein as a prognostic marker capable of refining the risk assessment of patients with molecular subtypes without specific molecular profiles (namely, the TCGA molecular subtype CN-L).
15
Similarly, Asmerom et al. demonstrated that FGFR2c expression was significantly associated with shorter progression-free survival in mismatch repair-deficient and p53 wild-type patients (namely, TCGA molecular subtypes MSI and CN-L), suggesting that its integration with molecular subtypes could increase prognostic accuracy.
16
These findings underscore the clinical relevance of TCGA subtypes while emphasizing the need for additional biomarkers to address their inherent limitations. Our study aligns with these efforts by identifying PEA15 as an independent risk factor for recurrence in early-stage EC. By integrating autophagy-related genes such as
The
Despite these findings, our study has inherent limitations. The retrospective design and lack of TCGA molecular subtyping in our clinical cohort restrict the ability to characterize the prognostic performance of
Conclusions
Our findings identify the autophagy-related gene
Supplemental Material
sj-docx-1-jbm-10.1177_03936155251383945 - Supplemental material for The autophagy-related gene PEA15 is a potential prognostic biomarker for
early-stage endometrial carcinoma
Supplemental material, sj-docx-1-jbm-10.1177_03936155251383945 for The autophagy-related gene
Supplemental Material
sj-tar-2-jbm-10.1177_03936155251383945 - Supplemental material for The autophagy-related gene PEA15 is a potential prognostic biomarker for
early-stage endometrial carcinoma
Supplemental material, sj-tar-2-jbm-10.1177_03936155251383945 for The autophagy-related gene
Footnotes
Acknowledgment
Ethics approval and consent to participate
Author contributions
Funding
Declaration of conflicting interests
Availability of data and materials
Supplemental material
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
