Abstract
Introduction
Pathologic conditions of hard tissues require fixative and replacement reconstruction therapies involving the use of medical implanted appliances, femoral head implants, and bone screws1,2 as well as the application of dental prostheses, such as dental crowns and root-formed dental implants. During the past several years, a number of materials, such as metals, ceramics, polymers, and their composites, have been used for the fabrication of these medical devices. Criteria such as an acceptable mechanical behavior and biocompatible chemical composition to avoid adverse tissue reactions have been used to define an ideal implanted material for medical and dental applications.
A wide range of biocompatible materials have been used in patients. Different biomedical applications require different properties of materials, including physical, mechanical, chemical, and biochemical properties. Among these, ceramics have been used widespread for medical device fabrication. The most commonly used ceramics are hydroxyapatite (HA) and tricalcium phosphate. They exhibit excellent biocompatibility due to their chemical and structural similarity to the mineral phase of native human hard tissues, ie, bone, tooth enamel, and dentine. However, their clinical applications are limited because of their brittleness and difficulty of shaping for implantation. Among biocompatible ceramics, zirconia-based biomaterials have gained attention as a biomaterial for reconstruction of hard tissues due to their superior mechanical properties and good chemical and biological compatibilities. Exploration into zirconia as a biomaterial began in the 1960s, 3 with most of the work over the years focused on the use of zirconia in orthopedics, specifically in the area of femoral heads for total hip replacements.4,5 This review focuses on the types of zirconia, advantages of zirconia-based biomaterials for bone and dental tissue reconstruction, responses of tissue and cells to zirconia, and surface modification methods for enhanced bioactivity of zirconia-based biomaterials. Current and future applications of zirconia-based biomaterials for hard tissue reconstruction, ie, osteogenic scaffolds and medical/dental implants, are also discussed.
Zirconia-Based Biomaterials
Zirconia has recently become one of the most popular ceramic materials in health care practices due to its improved mechanical properties, high biocompatibility, and aesthetics. 6 Zirconia is a compound consisting of 2 elements, ie, zirconium (Zr) and oxygen (O) in dioxide form. Zirconium is a transition metal element with atomic number of 40, atomic weight of 91.22, and density of 6.49 g/cm3. Pure zirconium can be found in both crystalline and amorphous forms. In nature, zirconium does not occur in a pure state but can be found in crystalline dioxide form (ZrO2) in minerals baddeleyite and zircon or conjugated with silicon oxides (ZrO2 XSiO2).7–10
Pure zirconia exhibits a phenomenon called “allotropy” which possesses different crystallographic phases due to altered atomic arrangement. Theses phases include monoclinic (M) phase, a deformed prism with parallel sides; tetragonal (T) phase, a straight rectangle prism; and cubic (C) phase, a square side straight prism. These dissimilar crystal structures are determined by the temperature. The monoclinic phase, which is stable at room temperature up to 1170°C, has inferior strength; the tetragonal phase is stable between 1170°C and 2370°C with superior mechanical properties; above 2370°C, the cubic phase is stable; and the material starts to melt at 2680°C.11–14 Zirconia phase transformation is martensitic transformation which is athermal, diffusionless, and associated with the shift in lattice position less than interatomic distance. The transformation results in volumetric change which is about 2% to 3% in case of the cubic to tetragonal phase transformation and approximately 3% to 5% for the tetragonal to monoclinic phase transformation. 10
Phase Transformation of Zirconia
As mentioned earlier, pure zirconia can be found in 3 crystallographic forms depending on the temperature: monoclinic—at room temperature, up to 1170°C; tetragonal—at temperature between 1170°C and 2370°C; and cubic—above 2370°C to 2680°C which is its melting point. On cooling, the tetragonal phase transforms to the monoclinic phase along with a substantial 3% to 5% increase in volume, resulting in residual stress and cracks which sufficiently lead to catastrophic failure. This transformation begins at 950°C and is reversible.8,15,16
Zirconia is considered to be a “ceramic steel,” which was first described by Garvie et al 17 after they found the phenomenon called “phase transformation toughening” in the calcia-stabilized zirconia. The rationale behind this phenomenon was first to stabilize the tetragonal phase of zirconia after sintering by additional dopants or stabilizing oxide agents (eg, CaO, MgO, and Y2O3). Sintered bodies of the tetragonal phase zirconia can be retained down to room temperature even though the equilibrium phase is monoclinic. Pure zirconia alloying with lower valance oxides results in an increase in more tetragonal and cubic phases and a decrease in the amount of the monoclinic phase at room temperature. These stabilized cubic and tetragonal phases have the same lattice structure as in the pure zirconia but have dopant ions substituted on Zr4+corners, with an oxygen vacancy sites to maintain the charge neutrality. However, the tetragonal phase remains metastable and can then transform to the more stable monoclinic phase under externally applied stress. The volumetric change will act in the opposite direction against the crack propagation, resulting in an improvement in strength and fracture toughness which exceeds the strongest alumina ceramic at that period.8,18
Transformation Toughening and Aging
Two major properties that affect lifetime of the zirconia include resistance to crack propagation (by the effect of transformation toughening) and hydrothermal aging (low-temperature degradation [LTD]). Phase transformation toughening, which improves zirconia mechanical properties, can be achieved when the tetragonal phase is metastable. In other words, tetragonal grains are able to transform under stress to stable monoclinic grains. However, without stress, this metastable tetragonal phase at the material surface can transform with water or humidity contact, such as body fluids. This phenomenon was first described by Kobayashi et al 19 and is known as “aging” or “LTD.” It has been reported that 3% mol yttrium-doped tetragonal zirconia polycrystal (3Y-TZP) femoral heads processed under autoclave sterilization fail after 1 to 2 years in vivo. 20
Both phase transformation toughening and aging occur together. This is like a 2-sided sword: the positive side is the stress-induced transformation to enhance mechanical properties, whereas the negative side is that the surface transformation introduces grain pull up, roughening surface, and initiating cracks. 21 Processing zirconia ceramics that are able to transform under stresses but with the resistance to aging with water is at stake. It becomes quite clear that the Y-TZP for orthopedics might not have been an option. 20
Type of Zirconia
Zirconia can be categorized into 3 main types, depending on dopants and its concentration, and the temperature of processing 17 :
Partially stabilized zirconia (PSZ) ceramics;
Tetragonal zirconia polycrystals (TZPs);
Zirconia-dispersed ceramics.
Zirconia dopants
Dopants or metal oxides used for stabilizing the tetragonal or cubic phases of zirconia can be classified according to the valence of cation and solubility in zirconia lattice. Commonly used divalent cations are calcium and magnesium, which possess low solubility. These dopants generally form tetragonal grains in the cubic matrix called PSZ.10,21 In PSZ, there is no more phase transformation toughening due to transformed tetragonal after cooling. Yttrium is the most used trivalent cation, and in certain applications, scandium, gadolinium, gallium, and iron can also be used. These trivalent cations give rise to either TZPs or PSZ ceramics depending on the processing and temperature. Tetravalent dopants such as cerium and titanium have the high solubility and stabilize tetragonal phase to form TZP ceramics. These tetravalent dopants improve the aging resistance but impair mechanical properties due to higher phase stability. 21
Decreasing “oxygen overcrowding” around zirconium cations through the introduction of oxygen vacancies, 22 which is the weak spot of the lattice, or through the expansion of the cation lattices, is how most stabilizers work. One of the major difficulties in processing and using zirconia ceramics is maintaining the delicate balance between the tetragonal phase stability necessary to prevent aging and the tetragonal phase transformability necessary for phase transformation toughening. The tetragonal phase can be stabilized at room temperature but is readily transformable under applied stress, whereas the absence of oxygen vacancies will prevent the occurrence of aging.
PSZ ceramics
In 1975, calcia-stabilized (Ca-doped) zirconia was claimed to be the first material in the history to have phase transformation toughening. 17 Then, magnesia-stabilized (Mg-doped) zirconia was started to be used in orthopedics. In PSZ, tetragonal or monoclinic zirconia nanometric precipitates are embedded in cubic zirconia matrix. A high concentration of yttria (>4% mol) can be found in PSZ form by high temperature treated and special cooling. Partially stabilized zirconia ceramics have lower strength compared with 3Y-TZP but considered as an alternative due to higher toughness 20 and resisted to aging. 23 Roy et al 24 showed that Mg-PSZ prostheses retrieved from femoral heads do not show any sign of aging after 5 years. Mg depletion can occur after water exposure at 200°C, resulting in tetragonal to monoclinic transformation at the surface.25,26 In dentistry, the yellow-orange color of Mg-PSZ also compromised the popularity for dental crown and bridge fabrication.
Tetragonal zirconia polycrystals
Monolithic tetragonal phase is another name for TZPs. Even though phase diagram and the sintering protocols for Y-TZP dictate that cubic phase should be a secondary phase, in most Y-TZP and Ce-TZP, tetragonal phase is considered the major or only phase. The Y-TZP is of special interest, as this is used for femoral prosthesis heads and, more recently, of dental prostheses such as crowns and bridges. Essentially, after the original work on PSZ, most of the practical knowledge on phase transformation toughening and on aging has been acquired on Y-TZP. 24
In general, 3Y-TZP acquires combination of strength and toughness among oxide ceramics, as a direct benefit of fine grain size and transformation toughening (Figure 1). Despite all these advantages, this material lacks resistance to aging. Ce-TZP (10%-12% mol yttria-doped) also has large grain size and inferior hardness and strength compared with those of Y-TZP. 21 In contrast, in tetravalent dopant–stabilized zirconia, tetragonal phase is able to transform to monoclinic phase under stress but resists to aging.

Scanning electron micrographs of 3% mol yttria-doped tetragonal zirconia polycrystal grain at different magnification: (A) ×10 000 and (B) ×20 000.
Zirconia-dispersed ceramics
These dispersion-toughened materials, such as ZrO2-toughened alumina (Al2O3), have been termed zirconia-toughened alumina (ZTA). 21 Adding transformable zirconia tetragonal phase in a nontransformable matrix is a possible option. Partially stabilized zirconia ceramics may be considered as one of these composites; the nontransformable matrix is made of cubic zirconia. The most used matrix is alumina and tetragonal zirconia particles are embedded in the alumina matrix. This is also called ZTA.
In such composites, the zirconia phase must be stabilized in the tetragonal phase. Yttria and ceria are the most used dopants/stabilizing oxides to stabilize the tetragonal phase. 8 Another approach is that pure zirconia particles can be stabilized within a high-stiffness alumina matrix. The composites can then be highly resisted or insensitive to aging. 20 The stability of the tetragonal phase is not easy to control: too small tetragonal zirconia particles will not transform under stress, resulting in impaired mechanical properties of the composites.
Advantages of Zirconia-Based Biomaterials for Hard Tissue Reconstruction
Improved material strength
As mentioned above, stabilization of zirconia ceramics can be achieved by alloying pure zirconia with other dopants, and consequently, the tetragonal phase can be partially stabilized at room temperature even though the equilibrium phase is monoclinic. Compared with alumina ceramics, these metastable tetragonal ceramics exhibit higher strength and exceptional fracture toughness when the transformation toughening is triggered by stress from crack tip. Transformation from a tetragonal phase to a monoclinic phase is associated with 3% to 5% volume expansion, resulting in compression of crack tip, inhibition of crack propagation, and enhancing fracture toughness. The Y-TZP exhibits high flexural strength (900-1200 MPa) and fracture toughness (9-10 MPa m0.5).27,28 In dental tissue replacement, high-strength Y-TZP has been used as root canal posts, 29 frameworks for all-ceramic crowns and fixed dental prostheses (FDPs), 30 custom-made bars to support fixed and removable dental prostheses, 31 implant abutments, 32 and dental implants. 33
Enhanced aesthetic
During dental restoration, especially in an anterior maxilla region, the color of tooth being replaced is a critical issue. The Y-TZP, that has superior optical property compared with that of metallic framework, is used very popularly in dental restoration, but it is still too white and opaque. Because the aesthetic demand of patients requiring a ceramic restoration is to be harmonized with the adjacent natural teeth, the translucency is one of the key for successful factors for dental restorations. Zirconia-based ceramics have poor translucency according to the amount of crystalline density, chemical nature, and the sintered density which determine the amount of transmitted, reflected, and absorbed light. Most of the light passing through it is intensely scattered and diffusely reflected, leading to its opaque appearance. 34 Some studies suggested that light transmission could be enhanced by microcrystals and full densification.35,36 Jiang et al 37 found that Y-TZP could gain nearly full density and high transmittance if sintering temperature is 1450°C to 1500°C. Coloring agents were also introduced to mimic natural color of teeth by adding coloring oxides to zirconia powder before or after sintering. Color can be customized involving infiltration of the machined restoration at the presintering porous stage to produce work pieces of various shades. 38
High biocompatibility
Biocompatibility refers to the ability of a biomaterial to perform its desired function with respect to a medical therapy, without eliciting any undesirable local or systemic effects in the recipient or beneficiary of that therapy, but generating the most appropriate beneficial cellular or tissue response in that specific situation, and optimizing the clinically relevant performance of that therapy. 39
Zirconia is considered as a biocompatible material, and no cytotoxic effect for zirconia ceramic has been shown in several cell types when tested both in vitro and in vivo.27,40 It has been reported that several ceramics including zirconia show no cytotoxicity to gingival fibroblasts. 41 Josset et al 42 investigated human osteoblast behavior in culture with zirconia discs, and they found that the osteoblasts showed good adhesion and spreading properties and the cells preserved their capacity to proliferate and differentiate into osteogenic pathways. The scanning electron microscopic results from our laboratory also support the cytocompatibility of zirconia for preosteoblasts and monocyte/macrophage cells (Figure 2). Scarano et al 43 examined the bond response to zirconia implants inserted into tibia of rabbits when the implants were retrieved after 4 weeks. They reported an evidence of new bone formation and osteoblasts directly on zirconia implants with no observable inflammatory responses. 43 Biocompatibility of zirconia may be attributed to good hydrophilicity and protein adsorption. It has been shown that albumin, a cell adhesion–inhibiting protein, is adsorbed more quickly than fibronectin, a cell adhesive protein, onto titanium. Moreover, albumin adsorption rate to titanium was more rapid than that to zirconia. This supports the notion that zirconia is highly biocompatible and is at least comparable with titanium. 44
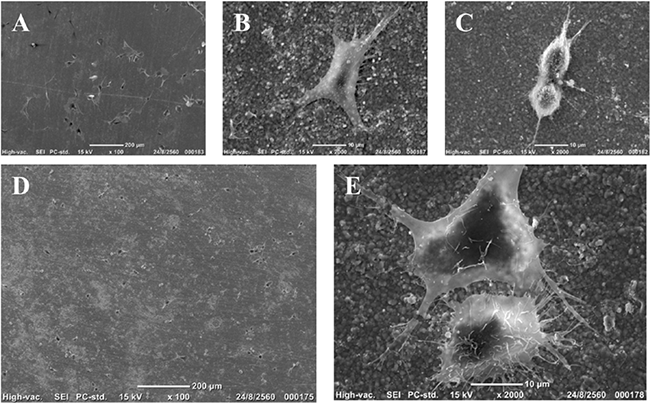
(A-C) Scanning electron micrographs of MC3T3-E1 preosteoblasts and RAW 264.7 monocyte/macrophage cells grown on zirconia for 24 hours. A and D show micrographs at low magnification, whereas B, C, and E show micrographs at higher magnification. Note that well-spreading cells with cytoplasmic projections, resembling filopodia are shown in B and E, and dividing cells are presented in C, suggestive of a highly cytocompatible surface.
It has been suggested that zirconia is unlikely to generate mutations of the cellular genome. 45 In particular, mutant fibroblasts found on zirconia were fewer than those obtained with the lowest possible oncogenic dose compatible with survival of the cells. 46 Moreover, zirconia causes less phlogistic reaction in tissue than other restorative materials, such as titanium. 47 This result is also supported by a study on peri-implant soft tissue around zirconia healing caps compared with that around titanium healing caps. Inflammatory cell infiltration, microvessel density, and the expression of vascular endothelial growth factor were found to be higher around the titanium caps than around the zirconia caps. 48
Less bacteria adhesion
Bacterial accumulation is known to correlate with extensive bone loss around implanted biomaterials. Bacterial adhesion shows a direct positive correlation with surface roughness. Other surface characteristics also seem to be of importance regarding bacterial biofilm formation. Different bacterial adhesion affinities have been reported for different biomaterials. Surface wettability and roughness may influence the adhesion of bacteria on biomaterials. Bacteria adhesion also depends on the bacterial species and biomaterial surface properties. For example, while hydrophilicity is the predominant factor for
Enhancement of bioactivity of zirconia by surface modification
Following placement of a biocompatible material, including zirconia, in the body, the tissue responds to the implanted material surface by allowing water molecules to interact with the surface 53 and subsequently forming an adsorbed protein layer.53,54 This allows cellular adhesion, migration, and differentiation, which occurs from a few hours to several days after implantation. 55 It is noteworthy that the cell-protein–bound surface interface occurring from as short as minutes after and up to days following biomaterial placement is of paramount importance for successful bone regeneration. This stage is tightly regulated by a wide range of biological factors, including extracellular matrix proteins, cell surface–bound, and cytoskeletal proteins, by chemical characteristics and topographies at the biomaterial surface, and by the released ions/products from the grafted material. 56 The ongoing development of surface modification methods of biomaterials for bone reconstruction, including zirconia, is therefore aimed to minimize such effects as well as to promote rapid wound healing and osseointegration of the grafted material.
A number of approaches have been considered in an attempt to achieve rapid and long-term success of osseointegrated zirconia-based biomaterials. Surface modification of either topography or chemistry, such as particle blasting, acid etching, oxygen plasma, UV treatment, and a combination of these treatments, greatly influences the surface bioactivity of zirconia. These include surface hydrophilicity, protein adsorption, osteoconduction (such as cellular attachment, spreading, and proliferation), and osteoinduction (such as osteogenic differentiation and mineralization). A recent study on the effect of acid etching reported that rough zirconia surface could effectively be prepared by acid etching pretreatment following glass infiltration and the resulting zirconia surface showed considerably enhanced favorable osteoblast responses. 57 In addition, when compared with the well-accepted biomaterial titanium surface, modified zirconia mediates a prominently stronger effect on the adhesion, proliferation, and differentiation in osteoblastic cells. 58 Influence of microstructured yttria-stabilized zirconia with surface modification by sandblasting, acid etching, heat treatment, and combinations on primary human osteoblast responses was also reported by Bergemann and colleagues (2015) 59 . Their results suggest that the yttria-stabilized zirconia possessing certain topographically modified surface show promising biological responses. Micro- and nanotopographies on zirconia by alumina blasting and hydrofluoric acid etching have been suggested to be a promising surface of enhancing favorable responses of osteogenic cells. 60 Noro et al 61 investigated surface characteristics and bioactivity of zirconia with modified surface topography (produced by alumina blasting and acid etching with hydrofluoric acid) and modified surface physicochemistry (modified with oxygen plasma, UV light, and hydrogen peroxide treatment), and the results showed that modification of surface topography or physicochemistry, especially of blast/acid etching as well as oxygen plasma and UV treatment, significantly augmented the surface hydrophilicity, resulting in superhydrophilicity. A notable reduction in carbon content and the substitution of hydroxyl groups may contribute to the reported superhydrophilicity. The resulting enhanced hydrophilicity of the modified zirconia is also sustainable, even with an aqueous solution storage following surface modification, a key consideration in translating into clinical application. 61 Wu et al modified the surface of zirconia using an oxygen plasma treatment which resulted in an enhanced and stable wettability zirconia surface. Such improved wettability of zirconia has also been shown to promote the attachment, proliferation, and osteogenic differentiation of human osteoblast-like cells. 62 Moreover, modification of biomaterial surface by osteogenic short-peptide immobilization has been suggested to enhance osteoconduction and osteoinduction of biomaterials for bone regeneration.63,64 It has also been shown that immobilization of a short protein peptide on the nanostructured cubic zirconia surface is achieved with a magnitude of adsorption energy higher than that on the atomically flat (smooth) surface. The strong electrostatic interactions are a major contributing factor in the enhanced adsorption immobilization at the nanostructured surface. It has been reported that the best electrostatic and steric fit of the protein to the inorganic surface corresponds to a minimum of the adsorption energy determined by the noncovalent interactions. UV pretreatment has also been reported to increase the bioactivity of zirconia-based materials, in terms of cellular attachment, proliferation, and eventually in vitro mineralization by fully active osteoblasts.65,66 This is attributed to the finding that UV treatment decreases the amount of surface carbon and converts the hydrophilicity status from hydrophobic to superhydrophilic. 65 Taken together, certain surface-modified zirconia-based biomaterials are likely to be one of the materials of choice for dental/medical implants for hard tissue reconstruction.
Current and Future Applications of Zirconia-Based Biomaterials for Hard Tissue Reconstruction
Medical implants
Zirconia offers high fracture toughness and flexure strength and is therefore one of the most fracture-resistant ceramics. Zirconia has been introduced to replace alumina in orthopedic uses with superior wear resistance because poor fracture toughness of alumina results in the unfavorable release of wear particles. To resolve some disadvantages of pure zirconia (ie, instability and phase transformation, leading to changes in shape and volume), stabilizing materials, such as magnesia (magnesium oxide), quicklime (calcium oxide), and yttria (yttrium oxide), are added. Controlled phase transformation is used to develop different zirconia composites for medical/orthopedic applications. These include TZP ceramic, which is the strongest and toughest zirconia-based ceramic with optimal material density and fine grain size. In addition, Y-TZP became a promising alternative structural ceramic because of its higher fracture toughness and strength. 8 Mixed composites of ZrO2 and Al2O3, known as ZTA, are also used successfully in hip replacement. 67 Zirconia-toughened alumina is a 2-phase biomaterial manufactured of zirconia particles dispersed in a dense, fine-grained alumina matrix. However, ZTA is still unstable, as it derives its strength and toughness from the mechanism that resulted in catastrophic failure of the zirconia-based medical materials. 68 Zirconia-toughened alumina achieve its properties through phase instability of the material itself. However, the instability of zirconia is exacerbated by human body temperature and moist environment. As zirconia transforms, its strength and toughness are reduced and over time the mechanical performance is just comparable with conventional alumina. A significant amount of work is clearly required to solve this limitation of zirconia-based materials.
Dental prostheses
Since early 1990s, zirconia has been used as substructures to support veneering ceramic materials for dental restorations. Most clinical failures reported in the literature 69 were fractures of veneering porcelain system with the rate of 2% to 9% for single crowns after 2 to 3 years and 3% to 36% for multiple-unit dental restorations after 1 to 5 years.70,71 New innovations are focusing on improving veneering technique by alternating manufacturing process of veneer using computer-assisted design and computer-assisted manufacturing (CAD/CAM) and modified sintering protocol. However, modifying veneering technique has not been very popular. 72
Recently, monolithic zirconia or full-contour zirconia restoration has been introduced to avoid using veneering ceramics as an alternative way. 38 The fracture resistance of monolithic zirconia has been reported by many authors. Preis et al 73 studied fracture resistance of 3-unit zirconia-based FDPs under different conditions. The median fracture force ranged from 1173.5 to 1316.0 N without statistical differences between groups, suggesting that full-contour zirconia FDPs might be considered as an alternative treatment option due to their high resistance to fracture. Zesewitz et al 74 investigated different single monolithic all-ceramic crowns including monolithic zirconia crowns, monolithic lithium disilicate, and monolithic feldspar ceramics. Monolithic zirconia crown exhibited the highest fracture resistance of all the samples studied under loading. The highest mean fracture load was reported as 5620 N for zirconia crowns.
New-generation zirconia with outstanding translucency for highly aesthetic restorations requires no porcelain veneer buildup. Increasing yttria concentrations may result in an increased cubic phase and an improved optical property (Figure 3). Optical property is a major challenging issue; composition, sintering protocol, and addition coloring liquids can be used for enhancing translucency. Beuer et al 75 showed that the light transmission of the polished zirconia full crown was significantly higher than that of glazed and veneered zirconia. In another study, Ilie and Stawarczyk 76 compared the amount of light transmission through monolithic zirconia, conventional zirconia, and glass ceramics and reported that the zirconia was less translucent than the conventional glass ceramic and the translucency decreased with increased thickness of materials. Although, recently, the translucency of zirconia has been improved, it is still not comparable with that of glass ceramics. The results from the studies also indicate that care should be taken in selecting the shade and polymerizing modes.

Scanning electron micrographs of high yttria-doped tetragonal zirconia polycrystal grain at different magnification: (A) ×10 000 and (B) ×20 000.
Future development of zirconia-based materials to gain more light transmission is challenging and can enhance the treatment result for the patients. “Aging-free” zirconia is an ideal goal but quite difficult to achieve because the transformation occurring during aging is a “natural” return to the monoclinic equilibrium state. One approach to avoid oxygen vacancies introduced by yttria doping is to select proper codopants such as tetravalent stabilizers or combined trivalent and pentavalent ions to minimize the vacancies required for charge neutralization. Nowadays, there are no commercially available zirconia-based materials that fulfill ideal properties. Fully free of aging, naturally translucent and phase-stable zirconia and its composites are options for the next decade.
Osteogenic scaffolds for hard tissue engineering
It has recently been reported that porous zirconia scaffolds may be fabricated by milling CAD/CAM blocks into the desired shape, and the HA-incorporated zirconia scaffolds possessed dramatically higher in vivo new bone formation volume. 77 This suggests that HA enhances osteogenic potency of porous zirconia/HA scaffolds. New bone formation can be observed at the pore cavity walls initially, followed by deposition of the entire pore volume. Islands of entrapped HA particles can also be observed in mineralized bone matrix. 77 Furthermore, new porous gradient HA/zirconia biomaterials can be prepared using foam-immersion, gradient-compound, and high-temperature sintering. These scaffolds can promote bone repair and support bone to grow into the scaffold pores. 78
Zirconia/HA scaffolds with different zirconia: HA ratios have also been fabricated, optimized, and extensively characterized. The porosity of a zirconia/HA scaffold can be adjusted from approximately 70% to 90%, and the compressive strength of the scaffold increases from 2.5 to 13.8 MPa when the zirconia content increased from 50 to 100 wt%. The biological responses in terms of cell adhesion and proliferation to the zirconia/HA scaffolds can be improved when compared with those scaffolds made from zirconia alone. Moreover, an in vivo study suggests that a stem cell–loaded zirconia/HA scaffold enhances bone regeneration around the implanted biomaterial. 79 In addition, zirconia/HA-based porous bioceramics loaded with recombinant human BMP-2 promote the repair of bony defect and facilitate bone growth in vivo, which might substitute the use of iliac bone grafts in routine clinical practice. 80 Taken together, zirconia-based scaffolds show good mechanical performances and biocompatibility and are promising biomaterials to be used in bone reconstruction needed in the treatment of load-bearing large bone defects.
