Abstract
Introduction
Dementia is a prevalent chronic condition affecting 55 million people globally, with particularly high prevalence among older adults. 1 Mild cognitive impairment (MCI) is often considered as an intermediate state between normal cognitive status in aging and early dementia, 2 and is a key stage in the prevention of dementia. Given that pharmacological interventions may cause side effects and their effectiveness remains to be fully evaluated, non-pharmacological interventions are receiving growing attention in the prevention and management of dementia in recent years. 1
Physical activity is defined as any bodily movement produced by skeletal muscles that results in the expenditure of energy. 3 It has been widely proved to be effective in improving cognitive function and slowing cognitive decline. 4 However, older adults with MCI/dementia often have a low level of physical activity and poor activity compliance. This may be attributed to cognitive decline, which can impair the ability to comprehend, remember, and execute instructions; reduce motivation and the capacity for behavioral change; and is frequently accompanied by declines in physical function.5,6 Systematically identifying the facilitators and barriers to physical activity participation in older adults with MCI and dementia can help develop scientific and effective management strategies to promote the physical activity participation in older adults with MCI/dementia, and the COM-B (Capability-Opportunity-Motivation-Behavior) model is a suitable framework for identifying the facilitators and barriers.
The COM-B model is a theoretical framework proposed by Michie et al., 7 and it is the core element of the Behavior Change Wheel (BCW) for understanding behaviors. Synthesized from 19 theories, this model is comprehensive and integrative. Additionally, it can be used in the beginning of a bottom-up strategy for designing interventions focused on behavior change. According to COM-B, physical activity participation in older adults with MCI/dementia is influenced by three core elements: capability, opportunity, and motivation, which may function independently or in combination. 7 For example, opportunities and capability can both influence motivation, and implementing a certain behavior can change capability, motivation, and opportunity in turn. There have been reviews using the COM-B model to summarize the facilitators and barriers to physical activity participation and exercise adherence in the general older population, and have shown satisfactory results.8,9
Scholars have also paid attention to and summarized the facilitators and barriers to physical activity participation in this special population, that is, the older adults with MCI and dementia. However, the original studies included in the latest review are as of 2019, 10 and a large number of new relevant original studies have appeared in recent years, so the evidence needs to be updated. In addition, factors influencing physical activity vary across different living environments and levels of cognitive impairment among older adults. For instance, physical activity levels in community-dwelling older adults may be influenced by determinants such as educational attainment and smoking habits. Conversely, physical activity levels among older adults residing in care facilities may be more affected by factors like reduced household chores and financial problem.11,12 Compared to individuals with MCI, older adults with dementia exhibit more severe cognitive impairment (such as executive function), greater decline in activities of daily living (ADLs), and have significantly prolonged sedentary time. 13 All of these can lead to differences in the factors influencing physical activity participation. Furthermore, different stakeholders prioritize distinct factors influencing physical activity. 14 For example, older adults with MCI/dementia place greater emphasis on health benefits and affective experiences. Informal caregivers not only focus on health benefits but also pay attention to the activity environment and the characteristics of the staff. Physiotherapy experts focus predominantly on physical state of older adults. 14 However, current reviews summarizing the facilitators and barriers to physical activity participation among older adults with MCI/dementia have overlooked heterogeneity attributable to living environments, cognitive impairment severity, and multi-stakeholder perspectives.
Therefore, the objectives of this review are as follows. First, summarize and update the facilitators and barriers to physical activity in older adults with MCI/dementia based on the COM-B model. Second, analyze the differences in the facilitators and barriers to physical activity participation in older adults with MCI/dementia across different residential settings, different levels of cognitive impairment, and different stakeholders’ perspectives. This study can assist healthcare professionals in identifying key determinants of physical activity and tailoring strategies for older adults with MCI/dementia, thereby providing a practical and evidence-based foundation for promoting physical activity participation in this population.
Methods
This systematic review is reported according to the latest Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines. 15 The review protocol has been registered in PROSPERO (CRD42024503022).
Search Strategy
The search period extended from the inception of the databases to January 20, 2024. Search terms encompassed key words related to cognitive disorder (eg, cognitive dysfunction, dementia, Alzheimer disease), words related to various physical activity (eg, exercise, sports, physical exertion) and the words related to influence factor (eg, barrier*, facilitat*, motivat*). We searched eight databases, including PubMed, EMBASE, PsycINFO, CINAHL, Cochrane Library, China National Knowledge Network, Wanfang Data and VIP. For specific search strategies, refer to Supplemental Material 1. In addition, references lists to the included studies and relevant reviews were retrieved to avoid omissions.
Eligibility Criteria and Study Selection
The inclusion criteria included the following: (1) participants: older adults with MCI/dementia, their caregivers, therapists, or other stakeholders; (2) intervention: any form of physical activity; (3) context: residing in community or care facilities (including nursing homes, hospital day centers and rehabilitation wards); (4) outcomes/aims: facilitators or barriers to the participation in any form of physical activity among older adults with MCI/dementia; (5) language was limited to English and Chinese.
Studies that met any of the following criteria were excluded: (1) conference abstracts, letters, research protocols, and dissertations; (2) physical activity was only part of various forms of activities; (3) older adults with MCI/dementia were only a subset of participants and were not analyzed separately; (4) full text was not available.
After deduplication of the retrieval results, two researchers independently screened and evaluated the title, abstract, and full text of each document according to the above criteria. Disagreements were resolved by consulting the third researcher.
Methodological Quality Assessment
Two researchers independently assessed the quality of the included studies. The Joanna Briggs Institute (JBI) Literature Critical Appraisal Tool 16 was used to assess the quality of the quantitative and qualitative studies. Specific assessment items were selected based on the corresponding study design. The overall quality of one study was expressed by the percentage of “yes” responses, with 60% and 80% as the cut-off values to distinguish low, medium and high quality. 17 The Mixed Methods Assessment Tool (MMAT) 18 was used to assess mixed methods studies. When more than 50% of the items were responded with “yes”, the study was considered high quality. 19 Any disagreements that arose during the methodological quality assessment were resolved by consulting the third researcher.
Data Extraction
The following information of the included studies were extracted: the first author and year, country, study design, setting, sample characteristics (sample size, diagnosis, age, gender), physical activity information, barriers and facilitators to physical activity participation. Data extraction was carried out by one researcher and checked by a second researcher, using predefined extraction templates.
Synthesis Methods
Barriers and facilitators to physical activity participation were integrated using the directed content analysis. 20 First, six themes (physical capability, psychological capability, reflective motivation, automatic motivation, physical opportunity and social opportunity) were pre-defined based on the COM-B model. Second, based on the definition of the themes, the findings were coded by two researchers independently. During the analysis, any codes that did not align with the six predefined themes were used to generate new themes. Finally, the codes under each theme were grouped based on relevance and then conceptualized into sub-themes.
In addition, to increase the precision and applicability of the results, subgroup analyses were conducted according to the type of residential setting, levels of cognitive impairment and the perspectives of different stakeholders.
Evidence Quality Assessment
Evidence from quantitative studies was assessed using the GRADE approach. 21 Evidence from qualitative studies was evaluated using the GRADE-CERQual approach. 22 The strength of synthesized evidence from both qualitative and quantitative sources was assessed based on the risk of bias, the consistency, quantity, and impact of the findings across studies. 23
Results
Study Selection
A total of 8555 articles were retrieved. After deduplication and title, abstract, and full-text screening, 33 studies were eligible for inclusion in the systematic review. Supplemental materials 2 shows all included original studies. Figure 1 summarizes the study selection process. Study selection flowchart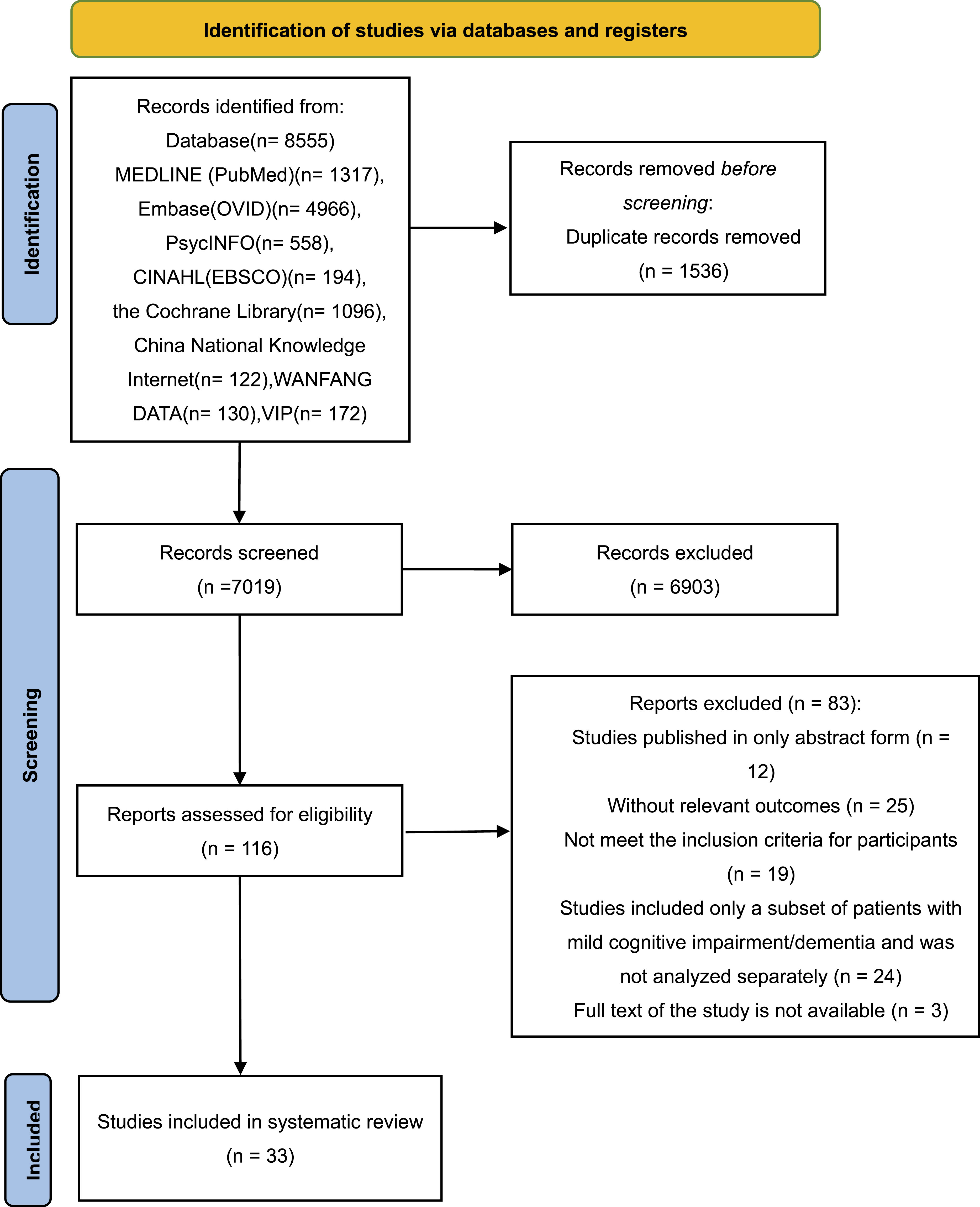
Study Characteristics
Characteristics of the Included Studies
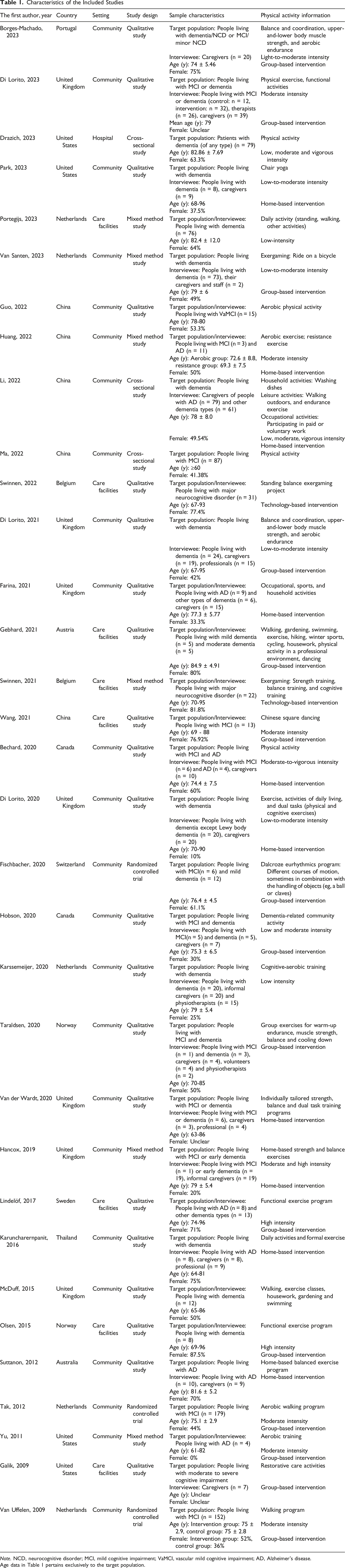
Age data in Table 1 pertains exclusively to the target population.
Methodological Quality
The percentage of “yes” ranged from 60% to 87.5%. 8 studies were of high quality, and 25 studies were of moderate quality, See Supplemental materials 3 for details.
Facilitators and Barriers to Physical Activity Participation in Older Adults With MCI/Dementia
Barriers and Facilitators Derived From Studies

Physical Capability
18 studies reported barriers related to physical capability, all categorized as physical mobility limitations. Regarding facilitators related to physical capability, 3 studies reported good mobility. Specific codes are presented in Table 2.
Psychological Capability
20 studies reported barriers related to psychological capability, including cognitive deficits (n = 15), behavioral and psychological symptoms (n = 8), inadequate knowledge of physical activity (n = 2), mental illness (n = 2) and lack of behavioral regulation ability (n = 2). 8 studies reported facilitators related to psychological capability, including memory support (n = 3), physical activity management skills (n = 5) and adequate knowledge of physical activity (n = 1). Specific codes are presented in Table 2.
Automatic Motivation
10 studies reported barriers related to automatic motivation, all categorized as lack of activity attractiveness. 16 studies reported facilitators related to automatic motivation, including positive feelings (n = 11), lifestyle habits conducive to physical activity (n = 5), and adequacy of activity attractiveness (n = 9). Specific codes are presented in Table 2.
Reflective Motivation
10 studies reported barriers related to reflective motivation, including perception of potential risk (n = 5), low self-efficacy (n = 4), negative physical activity experiences (n = 4), and the gap between ideal and perceived benefits of physical activity (n = 5). 18 studies reported facilitators related to reflective motivation, including positive physical activity experiences/negative inactivity experiences (n = 14), motivation from established goals (n = 9), and strong beliefs of physical activity participation (n = 7). Specific codes are presented in Table 2.
Physical Opportunity
18 studies reported barriers related to physical opportunity, including unfavorable physical activity environments (n = 14), time conflicts (n = 6), inappropriate organizational characteristics of physical activity (n = 6) and unfavorable material or human resources (n = 4). 22 studies reported facilitators related to physical opportunity, including appropriate organizational characteristics of physical activity (n = 16), favorable physical activity environments (n = 10) and favorable material resources (n = 6). Specific codes are presented in Table 2.
Social Opportunity
13 studies reported barriers related to social opportunity, including lack of support from relevant persons (n = 12), over-support from relevant persons (n = 5), and negative or pressure-inducing external evaluative factors (n = 3). 23 studies reported facilitators related to social opportunity, including explicit support from relevant persons (n = 22) and implicit support from relevant persons (n = 15). Specific codes are presented in Table 2.
Subgroup Analysis
Subgroup Analysis Based on Different Residential Settings

Subgroup Analysis Based on Different Stakeholders’ Perspectives

Certainty of Evidence
Of the 33 factors finally identified, 4 were of strong certainty and 29 were of moderate certainty (Details are shown in Supplemental materials 4, 5).
Discussion
Interpretation of Main Results
This systematic review comprehensively collated facilitators and barriers to physical activity participation in older adults with MCI/dementia based on the six domains of COM-B. The results indicate that the facilitators and barriers comprehensively involve the six domains of COM-B. In addition, the findings revealed variations across different residential settings types, levels of cognitive impairment, and stakeholders’ perspectives.
Compared with the recent umbrella review that identified 31 barriers and facilitators based the Theoretical Domain Framework (TDF), 10 This review further incorporated 23 recently published original studies, which accounted for 69.7% of the total number of studies included. In line with the umbrella review, it also found that the following four factors were most widely reported, namely explicit support from relevant persons, physical mobility limitations, appropriate organizational characteristics of physical activity, and unfavorable physical activity environments. The active participation of physical activity is directly related to environmental resources and social support, which runs through the whole process of starting and maintaining physical activity behavior. 27 Various physical mobility limitations often significantly alter the perception of physical activity in older adults, 9 so there is a need to provide personalized physical activity program guidance tailored to the physical status of older adults.
In addition, this review found some new barriers, including lack of behavioral regulation, low self-efficacy, the gap between ideal and perceived benefits of physical activity, and negative or pressure-inducing external evaluative factors. Behavioral regulation ability is the key to change from action decision making to actual behavior adoption, and it plays an important role in the process of behavior change.28,29 Therefore, the fundamental reason why unhealthy lifestyles hinder physical activity may be the lack of behavioral regulation ability. In older adults with MCI or dementia, the decline in cognitive function can lead to impaired executive function, 1 making it difficult for them to develop appropriate activity plans. This decline in psychological capability directly limits an individual’s ability to translate activity intentions into structured and sustained actions. From a neurological perspective, this may be linked to functional impairments in brain regions associated with cognitive control and memory, such as the prefrontal cortex and hippocampus,30,31 which hinder patients from forming and maintaining new behavior patterns that require cognitive effort. 1 Therefore, increasing participation in physical activity requires the support of cognitive-assistive strategies—such as simplified instructions and visual cues—to enhance their practical capability for behavioral execution.
In terms of low self-efficacy, it may lead to avoidance behaviors due to fear of failure or injury, such as refraining from going out, declining participation in group exercises, or even completely ceasing activities. 9 Older adults with MCI and dementia face confidence challenges due to loss of cognitive function. Hence, the negative impact of decreased self-efficacy on their physical activity participation may be greater than that in older adults with normal cognition. 32 In addition, there is already evidence showing that self-efficacy is positively correlated with both cognitive function and physical activity levels. 33 It interacts with the aforementioned psychological capability deficits and social negative evaluations, forming a vicious cycle: insufficient capability leads to experiences of failure, which lower self-efficacy 9 and may invite negative evaluations; such evaluations further undermine confidence and motivation, ultimately reinforcing sedentary behavioral patterns. The implication is that intervention strategies must include components to build mastery and confidence, such as graded tasks and positive feedback.
The gap between ideal and perceived benefits of physical activity is an important barrier. This is consistent with the results of Yu et al 34 The possible explanation for this is that dementia is a degenerative disorders, where even physical activity-induced cognitive improvements may be difficult to detect, or it may also be due to too little exercise or lack of self-comparison. 34 Furthermore, immediate negative feedback, such as physical discomfort or poorly designed activities, may further exacerbate this cognitive discrepancy. Such negative experiences could dominate behavioral decision-making by enhancing activity in brain regions like the insula, which is responsible for interoception and aversion processing, thereby overwhelming the prefrontal cortex-driven rational cost-benefit analysis and hindering the translation of reflective motivation into action. 35 Future interventions should focus on highlighting the immediate, perceptible positive benefits of physical activity, such as through the use of real-time feedback tools.
In terms of negative or pressure-inducing external evaluative factors, people are often affected by the past (cognitive normal period) and present “identity” of people living with dementia, and hold too high or too low expectations. 36 Too high expectations may cause negative emotions such as fear of disappointment, and too low expectations may cause stigma, which could reduce the physical activity participation. More importantly, these external evaluative pressures often directly undermine the autonomy of older adults in their daily activities. According to Self-Determination Theory, such impairment of basic psychological needs (such as autonomy) can further reduce their intrinsic motivation, and may even lead them to actively withdraw from social activities. 36 Therefore, when implementing promotion strategies, a focus can be placed on peer support programs. Specifically, it involves introducing older adult volunteers with similar experiences to serve as role models and foster a sense of identification, thereby counteracting the internalization of negative evaluations.
The findings of this study and the existing evidence discussed above are basically consistent with the assumptions of the COM-B model regarding the relationships among C, O, M, and B. That is, capability, opportunity, and motivation not only directly influence physical activity behavior individually, but capability and opportunity also indirectly affect physical activity behavior by influencing motivation. Furthermore, physical activity behavior in turn influences C, O, M. The repeated practice of a behavior is inherently a process of capability refinement. For instance, regular and consistent exercise can enhance cognitive functions such as memory (a psychological capability). 37 The authentic experiences derived from behavioral outcomes profoundly influence motivation. When physical activity yields sustained satisfaction and habits are established, it can enhance an individual’s autonomous motivation. 9 Additionally, engaging in the behavior may motivate individuals to actively seek environments consistent with that behavior, such as familiar community settings, 9 while also potentially attracting social support and resources from others, thereby further reinforcing and expanding existing opportunity structures. Conversely, the cessation of behavior may lead to the contraction of related opportunities. In the future, further research and validation are needed to elucidate the specific interactions among capability, opportunity, motivation, and physical activity behavior in older adults with MCI.
Interestingly, this review further observed differences in the facilitators and barriers to physical activity participation among older adults with MCI/dementia across different residential settings, levels of cognitive impairment, and stakeholders’ perspectives. In community settings, the emphasis is on the appeal of activities, involving benefits and preferences. In care facilities settings, the emphasis shifts to the influence of the staff (such as responsibilities) and environmental design of care facilities. This difference may be due to that care facilities usually have adequate and better-qualified professionals specializing in older adults, regularly organized activities, and centralized management, and the groups that live together are relatively stable and are prone to being influenced by others. 38 Conversely, the community setting offers greater autonomy, and the environments are more open and infrastructure-rich. 39 Therefore, physical activities need to be more attractive. In older adults with dementia, cognitive function performance, external influences, and support systems are important influencing factors of physical activity; whereas those with MCI emphasize staff characteristics. This differentiation may be attributed to the fact that dementia causes more severe cognitive impairment, 1 requires greater support, and is also more severely affected by social stigma. 40 While older adults with MCI preserve their functional independence and desire more positive environments. Regarding the perspectives of different stakeholders, older adults with MCI/dementia focus on internal/external activity conditions and motivation for activities. It is noteworthy that this population’s dependence on environmental support stems from increasing cognitive impairment, while cognitive decline also diminishes their ability to adapt to the environment. 41 Informal caregivers concentrate on their own beliefs about physical activity; and staff members focus on factors related to their work practices, such as the ability of participants to access and use digital support. Therefore, different stakeholder groups may uniquely consider the factors most relevant to themselves.
Strengths and Limitations
Based on the COM-B model, our systematic review provides a systematic analysis of the factors that promote and hinder physical activity in older adults with MCI/dementia by integrating the latest research results, and found several new meaningful factors compared with the previous reviews. This review also analyzed differences in these factors by types of residential settings, levels of cognitive impairment, and stakeholder perspectives. Despite these advantages, there are some potential limitations in this review. First, the majority of participants came from high-income countries, which may limit the diversity of views and experiences. Second, due to limited information and the large variations in physical activity regimens in the included studies, subgroup analyses could not performed according to the type of physical activity. Finally, Research targeting older adults with MCI remains relatively scarce, which may result in incomplete coverage of the facilitators and barriers specific to this population.
Implications for Research and Practice
Future research should further explore the facilitators and barriers to different types of physical activity among older adults with different level of cognitive impairment, so as to make intervention strategies more accurate. The evidence for older adults with MCI should be further supplemented. Low- and middle-income countries should be given more concern. In addition, according to the results of this study, future studies can further develop relevant intervention strategies based on BCW.
In practice, relevant caregivers should pay attention to identify the facilitators and barriers of physical activity in older adults with MCI/dementia, and select corresponding strategies to promote physical activity participation in this population. Furthermore, for older adults with MCI/dementia living in different residential settings, with varying levels of cognitive impairment, and for different stakeholders, the developed physical activity promotion strategies should vary in their emphases. In community settings, it is important to diversify highly engaging activity formats to organically integrate physical activity with social interaction. In care facilities, efforts should focus on optimizing the physical environment and activity organization models, while strengthening specialized training for staff. For those living with dementia, providing ample environmental cues, memory aids, and consistent positive reinforcement from caregivers and staff becomes crucial. It is essential to acknowledge the perspectives of different stakeholders. Interventions should equip informal caregivers with the knowledge and skills to offer balanced support (avoiding overprotection) while ensuring that staff receive adequate training in activity adaptation and digital support technologies.
Conclusion
The facilitators and barriers to physical activity among older adults with MCI/dementia comprehensively involve the six domains of the COM-B framework, which exhibit varying emphasis across different residential settings types, levels of cognitive impairment, and stakeholders’ perspectives. This evidence provides a foundation for developing future physical activity promotion strategies for this population.
Supplemental Material
Supplemental Material - Facilitators and Barriers to Physical Activity Participation in Older Adults With Mild Cognitive Impairment or Dementia: A Systematic Review Based on the COM-B Model
Supplemental Material for Facilitators and Barriers to Physical Activity Participation in Older Adults With Mild Cognitive Impairment or Dementia: A Systematic Review Based on the COM-B Model by Jiachen Han, Wan Sun, Xin Yin, Luo Wang, Fang Zhou, Shuo Wang in American Journal of Alzheimer’s Disease & Other Dementias®
Footnotes
Ethical Considerations
Consent to Participate
Author Contributions
Funding
Declaration of Conflicting Interests
Data Availability Statement
Registration
Supplemental Material
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.

