Abstract
Introduction
Pediatric arthritis poses a diagnostic challenge due to the wide range of potential underlying causes, including infectious, inflammatory, malignancy, and autoimmune conditions.1–6 Septic arthritis and systemic juvenile idiopathic arthritis (sJIA) are two important but distinct conditions that present with overlapping clinical features such as fever, joint swelling, and pain.3,6 Septic arthritis, especially in the hip joint, is an orthopedic emergency that requires prompt identification and treatment to prevent severe joint damage and long-term disability.1,5,6 In contrast, sJIA is an autoinflammatory disease characterized by systemic inflammation and multi-organ involvement and requires immunomodulatory therapy to achieve remission. 4
Differentiating between these two conditions is critical because misdiagnosis can lead to inappropriate treatment and significant delays in effective management. Septic arthritis often presents as acute monoarthritis, whereas sJIA can manifest as polyarthritis, persistent fever, and systemic symptoms.1,3,6 The similarity in presentation can confound clinical assessment, especially when the early diagnostic steps are inconclusive. Diagnostic accuracy is further complicated in pediatric patients, where symptoms may be nonspecific and physical examination findings can be challenging to interpret.5,6
This case report presents the case of a 3-year-old boy who was initially diagnosed with septic arthritis and treated accordingly but was later found to have sJIA. This case highlights the importance of considering a broad differential diagnosis in pediatric patients with persistent fever and arthritis, particularly when there is a lack of response to standard treatment. The discussion also emphasizes the role of a multidisciplinary approach in ensuring accurate diagnosis and effective management.
Case presentation
A 3-year-old boy presented with a 1-week history of high fever, particularly in the evening and at night, accompanied by pain in his ankles and knees.
Physical examination and laboratory findings
Upon admission to a general hospital, the patient exhibited arthritis in both knees and ankles, with high fever occurring in the evenings and at night, along with red macular rashes on the trunk and limbs that intensified during fever spikes. Ultrasound reports indicated effusion in both the hip and knee joints, as well as in the ankles. Laboratory tests revealed leukocytosis with neutrophil predominance, thrombocytosis, an estimated erythrocyte sedimentation rate (ESR: 95 mm/h), C-reactive protein (CRP: 75 mg/dL), and negative blood cultures.
Initial treatment
The patient was initially diagnosed with septic arthritis and underwent arthrocentesis and arthrotomy of both hip and knee joints (Figure 1). The patient was treated with ceftriaxone and vancomycin. Synovial fluid analysis revealed white blood cells (WBC <5000/mm3), neutrophils <40%, and negative synovial fluid smear and culture results. Despite the results of synovial fluid analysis and culture, the patient continued the initial treatment with antibiotics for 12 days before being transferred to the pediatric rheumatology department. The following figure illustrate the surgical procedure and post-operative management undertaken to alleviate joint effusion and inflammation.
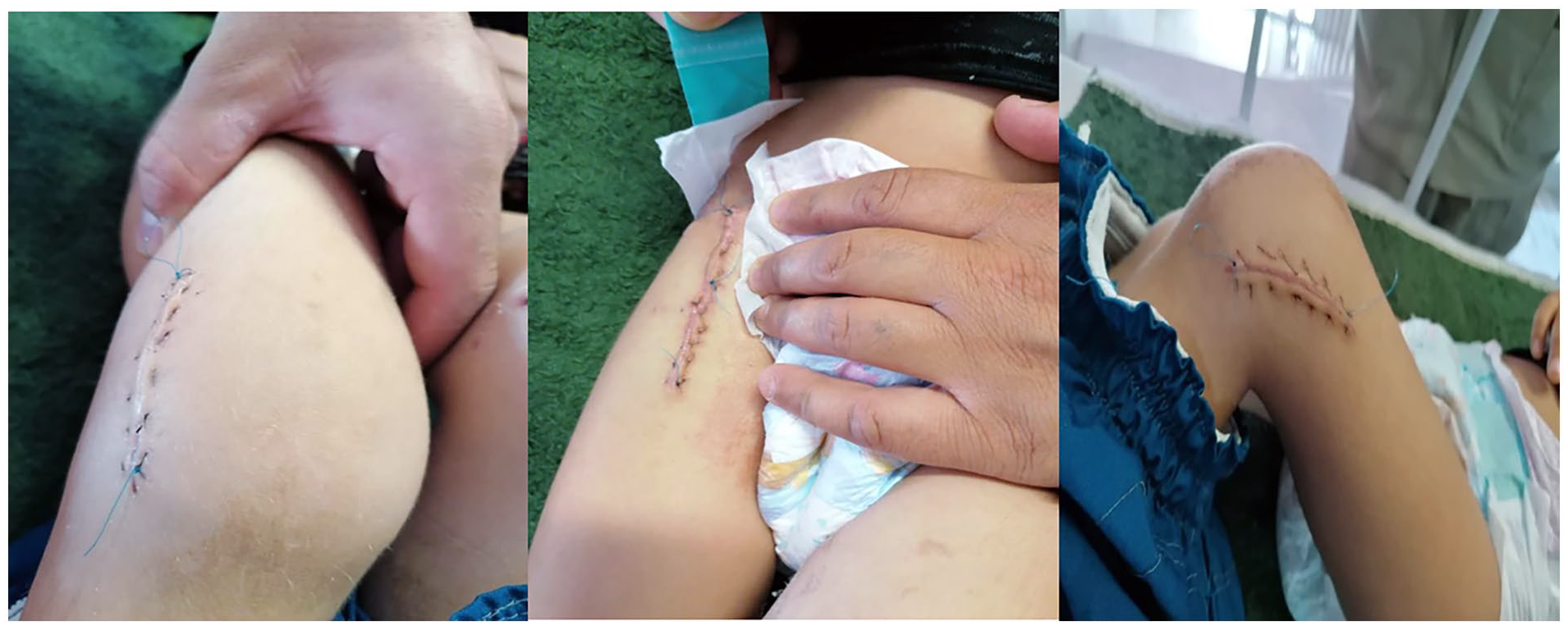
Post-arthrotomy images of the patient’s knees and right hip, showing the incision site following joint surgery. This procedure was performed to drain the synovial fluid and alleviate joint effusion as part of the initial management of septic arthritis.
Further evaluation and diagnosis
After the treatments for 12 days based on the diagnosis of polyarticular septic arthritis, the patient’s fever continued and the inflammatory factors increased. Therefore, the patient was sent to a children’s hospital. At the Imam Hossein Children’s Hospital, additional symptoms included salmon-colored rashes during fever spikes, hepatosplenomegaly, cervical and axillary lymphadenopathy, and pericardial effusion on echocardiography were noticed. Considering the spiking evening and nocturnal fever, rash incidence, and polyarticular arthritis persisting for 2 weeks, sJIA was suspected. Paraclinical data were requested, representing leukocytosis (WBC: 27,000/mm3), thrombocytosis (platelet: 750,000/mm3), neutrophilia (neutrophil ratio: 82%), ESR: 120 mm/h, CRP: 98 mg/dL, and ferritin: 750 mg/dL. Table 1 summarizes the patients’ laboratory results in the first month of illness (throughout hospitalization and after discharge).
The patients’ laboratory results in the first month of illness.

CRP: C-reactive protein; ESR: erythrocyte sedimentation rate; WBC: white blood cells.
Blood and urine cultures, brucellosis serology, cytomegalovirus antibodies, COVID-19 polymerase chain reaction, Epstein-Barr virus antibodies, and Parvovirus B19 serology were all negative. Rheumatological tests, including antinuclear antibody, angiotensin-converting enzyme, and antiphospholipid antibodies, were negative. Complementary tests, uric acid and lactate dehydrogenase levels, peripheral blood smear, and echocardiography results were normal. Bone marrow aspiration revealed normal findings, with no evidence of malignancy. Based on the clinical and paraclinical manifestations and ruling out other potential diagnoses according to the International League of Associations for Rheumatology (ILAR) criteria, sJIA diagnosis was confirmed.
Treatment and outcome
The patient was treated with methylprednisolone pulses (30 mg/kg/day) for three consecutive days, an oral suspension of ibuprofen (40 mg/kg/day), and methotrexate injections (15 mg/m² weekly). Four days after starting treatment, the patient’s fever resolved, inflammatory marker levels decreased, and arthritis improved. At the 4-week follow-up, the patient was able to walk without any signs of fever, lymphadenopathy, or arthritis, and laboratory tests showed normalized Aspartate aminotransferase (AST), Alanine aminotransferase (ALT), and inflammatory markers. Prednisone was tapered, and treatment with ibuprofen and methotrexate was continued. The patient has been in remission for 6 months.
Discussion
Arthritis in children can have various causes, including infectious, inflammatory, immunodeficiency, hematologic, and malignant origins. It is crucial to determine the underlying cause of arthritis when evaluating children with this condition. A proper diagnosis based on clinical and paraclinical findings must be established before initiating treatment. Acute septic arthritis in children, especially in the hip joint, is an orthopedic emergency. Usually, septic arthritis is in the form of monoarthritis or two adjacent joints, and it rarely occurs in the form of polyarthritis, for example, in severe sepsis. In addition, in septic arthritis, there is usually no involvement of other organs, rashes, or hepatosplenomegaly. These important issues were not considered in this case and caused a misdiagnosis.
Since the clinical presentation can be similar to that of other joint pathologies, acute septic arthritis is a diagnostic challenge. This is particularly true for infants and neonates, in whom refusal to feed, crying, and discomfort with joint movement limitations can be the presenting symptoms. Delays in diagnosis and inappropriate treatment can result in devastating joint damage, leading to lifelong disability. 5 Unfortunately, the diagnosis of septic arthritis is not always straightforward. For example, in hip arthritis, transient synovitis is a benign, self-limiting condition that mimics septic arthritis. Other less common orthopedic conditions can also be present and must be excluded.6,7
This case illustrates the potential for the misdiagnosis of septic arthritis in the context of sJIA. Given the overlapping symptoms between septic arthritis and sJIA, it is essential for clinicians to consider sJIA in the differential diagnosis, particularly in patients with oligoarthritis or polyarthritis, and when there is persistent fever despite appropriate antibiotic therapy.6–8 Other causes of polyarthritis, including malignancy, hematologic and metabolic disorders, and immunodeficiency, should also be considered in differential diagnosis. The early recognition and treatment of sJIA can prevent complications and improve patient outcomes.
Conclusion
This case highlights the diagnostic challenges associated with differentiating sJIA from septic arthritis, particularly in pediatric patients with overlapping clinical features. Early and accurate diagnosis of sJIA is critical because misdiagnosis can delay appropriate treatment and lead to complications that significantly affect patient outcomes. Clinicians should consider sJIA in the differential diagnosis of pediatric patients presenting with persistent fever and polyarthritis, particularly when standard treatments for septic arthritis fail. A thorough evaluation, including imaging, comprehensive laboratory analysis, and careful consideration of clinical presentation, is essential to ensure an accurate diagnosis and timely intervention. Collaboration across specialties, such as rheumatology and pediatrics, is key to effectively managing complex cases.
