Abstract
Introduction
Clinical education that integrates theoretical and practical learning components into a real-life situation should help provide a learning experience that promotes the acquisition of appropriate skills, behaviors, and attitudes for future professional practice (AlMekkawi et al., 2020). Nursing trainees benefit from effective clinical teaching, hence improving patient care quality (Hababeh & Lalithabai, 2020). Furthermore, nursing students benefit from clinical experience by participating actively in the healthcare team, seeking solutions to real-life problems, and learning by doing, helping them to become competent practitioners (Okoronkwo et al., 2013). Today's nursing students need to be adequately prepared for professional nursing practice in complex clinical settings. This requires clinical instruction and experience improvement to meet current practice standards (Hababeh & Lalithabai, 2020).
Clinical supervision is crucial to developing nursing students’ knowledge, skills, and professional attitudes. A clinical instructor is expected to be an excellent practitioner with great teaching skills that are responsible for ensuring that students learn how to apply theory, gain hands-on experience, practice techniques, and develop professional maturity (AlMekkawi et al., 2020). The characteristics of clinical instructors have a great impact on the professional training, socialization, and transition of students into their workplaces (AlMekkawi et al., 2020). Therefore, it is crucial to identify and provide feedback to them to cultivate appropriate and helpful characteristics in clinical instructors.
There has been growing attention to identifying the characteristics that make clinical instructors effective, such as professional knowledge, role modeling, competence, and communication skills, to facilitate optimal student learning (Madhavanprabhakaran et al., 2013). Moreover, exploring effective clinical instructors’ characteristics of nursing professionals’ effective teaching. Furthermore, a recent integrative review of the literature identified the main sources of insight into how to enhance educational programs for professional nursing development (Madhavanprabhakaran et al., 2013). Therefore, it is important to identify the characteristics of a good nursing clinical instructor.
Review of Literature
According to a previous study in Oman, nursing students rated the professional competence of instructors as the most important characteristic, followed by the instructors’ relationship with students. Among the top five most effective clinical instructor characteristics were objective evaluation, role modeling, clinical competency, and communication skills (Madhavanprabhakaran et al., 2013). Similarly, in a study conducted on respiratory therapy students in the southeastern metropolitan area of the United States, it was clarified that the findings highlighted that professional competencies and relationships with students were noted by the participants as the most important behavioral characteristics of the clinical preceptor. This aligns with a prior study in Oman (Aldhahir et al., 2020). This similarity indicates that these behavioral teaching characteristics are important, regardless of the study location or setting.
In the United Arab Emirates, it was found that the majority of students reported personality and teaching ability as the highest categories for an effective clinical instructor. The majority of faculty members reported interpersonal relations and nursing competence as the most effective behaviors (AlMekkawi et al., 2020). The study finding was consistent with a study in the Philippines, where Soriano and Aquino found that the majority of the students selected personality traits and interpersonal relations as the most effective behaviors, and faculty members selected nursing competence and teaching abilities as the most effective ones (Soriano & Aquino, 2017).
On the other hand, a study from Egypt revealed that teaching ability and interpersonal relationships were the most highly valued characteristics rated by both students and clinical educators, and both groups ranked the subset of nursing competence, personality traits, and evaluation as the lowest valued characteristic (Banan et al., 2017). Another comparative study among students and clinical educators also showed a consistent result in the ranking of effective clinical teaching characteristics, as interpersonal relationships, evaluation, and nursing competence ranked first, second, and third, respectively (Lee et al., 2002). This difference could be attributed to the variations in the socioeconomic status of the country, personal character, and environment.
Our study aimed to explore the characteristics of effective clinical instructors from the perspective of nursing students, faculty, and preceptors. Likewise, it is intended to identify which characteristics of effective clinical instructors are most important to them in all nursing programs in Saudi Arabia.
Methods
Study Design and Settings
A cross-sectional study was done utilizing a standardized questionnaire, the Nursing Clinical Teacher Effectiveness Inventory (NCTEI; Hababeh & Lalithabai, 2020), to explore the perception of effective clinical instructor characteristics among nursing students, faculty, and hospital preceptors in Saudi Arabia. The data collection process was conducted between April 2022 and September 2022.
In Saudi Arabia, nursing programs consist of 5 years of study, including a 12-month internship. The first year of the program introduces students to fundamental scientific principles through various science courses. During the second, third, and fourth years of the program, students study clinical courses that provide the opportunity to participate in patient care experiences on clinical days. In the fifth (last) year, students will undergo clinical training (internships) for 12 months. This is a focused compulsory training period for students whose goal is to ensure that the theoretical knowledge they have acquired during their university years is applied as effectively as possible in an actual setting.
Participants and Sampling Procedure
The study sample comprises nursing students, faculty members, and hospital preceptors who were approached using a non-probability convenience sampling technique. Nursing students across all academic levels were recruited in addition to nursing faculty members who are educators qualified to teach nursing courses and evaluate students’ learning. Furthermore, hospital preceptors are experienced nurses who supervise nursing students during clinical rotations to help students translate theoretical learning into clinical practice and develop clinical skills. We excluded students, faculty, and preceptors with no clinical training experience.
Participants were enlisted from various universities (for students and faculty members) and hospitals (for clinical preceptors) across Saudi Arabia and were invited to fill out an online questionnaire using Google Forms. The questionnaire was distributed through social media platforms, including WhatsApp, Telegram, Twitter (X), and participants’ personal or university email. Once the questionnaire had been filled out, respondents were instructed to submit the form to transfer the data into Excel for the intended use.
Before progressing to the survey, written consent was obtained, and participants agreed to participate of their own free will. Moreover, participants were informed about the purpose of the study, informed that they could withdraw at any time without providing a reason, and assured that their responses would not be disclosed and would be kept confidential.
Data Collection Tool
Data collection included socio-demographic information and the NCTEI (Hababeh & Lalithabai, 2020). The first section contained different socio-demographic information based on the participant's occupational level. Students’ demographic information included age, gender, academic level, and length of training (for interns only). Faculty and hospital preceptors’ demographic information included age, gender, highest degree, and years of experience.
The second section included the NCTEI, developed by Knox and Mogan (1985) as a survey instrument for nursing students, graduates, and faculty to rate the characteristics of the clinical teacher behaviors that they have encountered (Hababeh & Lalithabai, 2020). The adapted questionnaire had 47 items that were categorized into five major dimensions: teaching ability (17 items), nursing competence (nine items), evaluation (eight items), interpersonal relations (six items), and personality (seven items). The scale items were rated on a 7-point range of responses from 1 (
Statistical Analysis
Data management and analyses were performed using SPSS (Version 16.0, StataCorp LP, College Station, TX, USA). Demographics were presented as means (
Results
A total of 710 participants—510 students, 102 faculty members, and 103 hospital preceptors—were included in the analysis, as Table 1 illustrates. Nearly three-quarters of nursing students were enrolled in clinical training throughout their undergraduate studies, and the majority of them (79%) were female and between the ages of 21 and 25. Similar to the faculty, 49% of the holders of doctorates had more than 10 years of teaching experience, with 40.2% of them having done so. Regarding preceptors, 40.8% have 1–3 years of clinical experience, 68% have bachelor's degrees, and 5.9% have doctorates.
Demographic Information.

The overall means for each clinical teaching characteristic perceived by all participants are shown in Table 2. Evaluation was deemed the most effective clinical instructor characteristic (5.721 ± 1.25), whereas nursing competence was deemed the least important (5.642 ± 1.26).
The Domain Scores of Participants’ Perceptions of the Characteristics of an Effective Clinical Instructor.

A one-way ANOVA was performed to compare the mean difference of the effective clinical instructors’ subscales among the three groups (students, faculty, and preceptors). A significant difference was found between nursing students, faculty members, and preceptors in terms of perceptions of clinical instructor effectiveness across all subscales (Table 3). Faculty members perceived all clinical instructor characteristics as more important than preceptors and students, as shown in Table 3. Evaluation was perceived by both faculty members and preceptors as the most important characteristic (6.21 ± 1.170) and (5.98 ± 0.904), respectively, followed by interpersonal relationships (6.17 ± 1.205) and (5.88 ± 1.122), respectively. Nursing competence was perceived as the least important by faculty (6.07 ± 1.221), while personality was the least important to preceptors (5.80 ± 0.928). On the other hand, nursing students perceived interpersonal relations as the most important (5.57 ± 1.261), followed by teaching abilities (5.57 ± 1.231), whereas nursing competence was perceived as the least important (5.51 ± 1.298).
One-Way ANOVA Comparing Between Student
(

Upon assessing the clinical instructors’ characteristics across different academic levels, students do not differ in their perception, as shown in Figure 1.

Comparing the mean of all characteristics between students according to their academic level.
Faculty members with different years of teaching experience do not differ in their perception of effective clinical instructors’ characteristics (Figure 2).
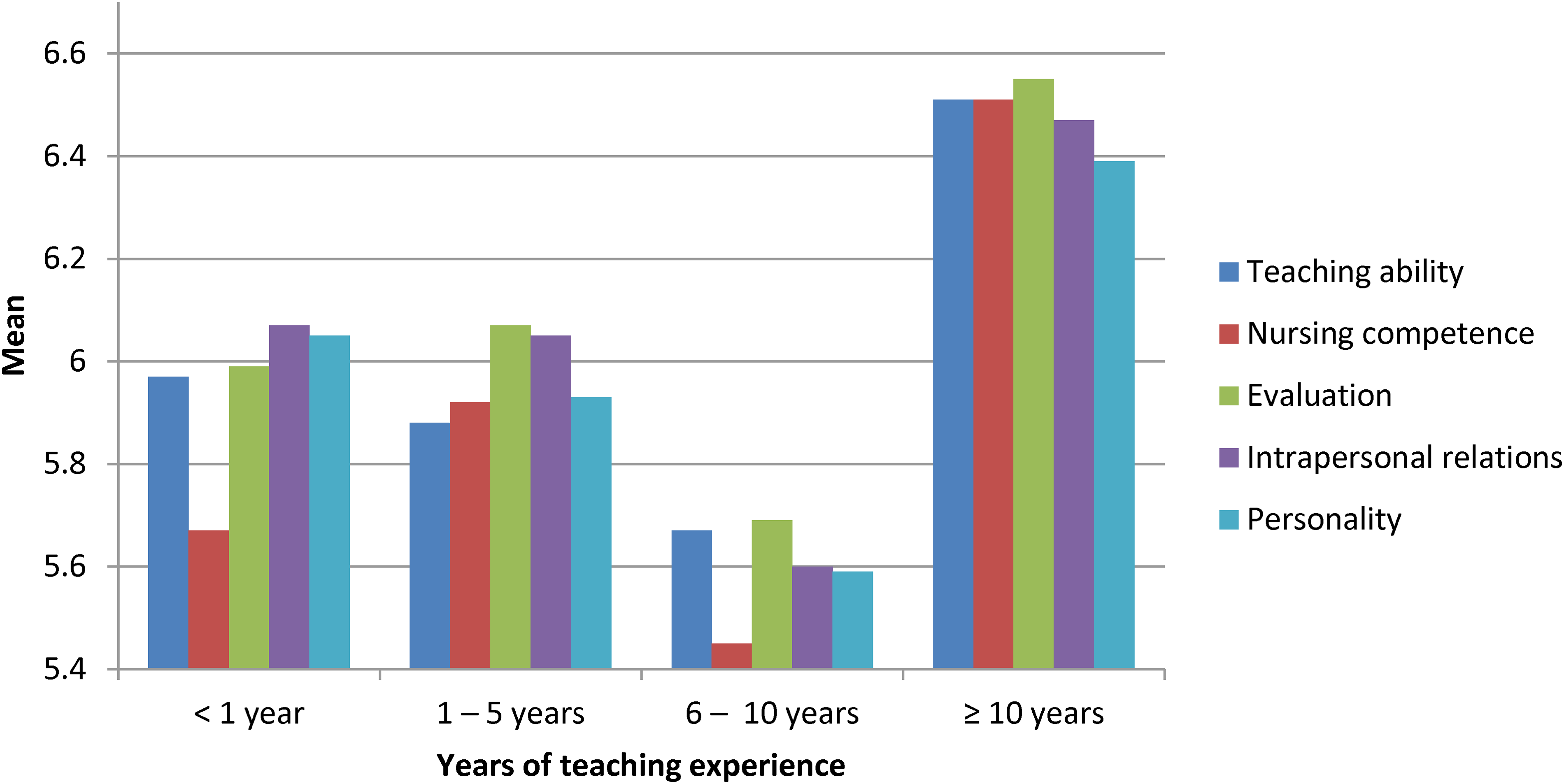
Comparing the mean of all characteristics between faculties according to their years of teaching experience.
Preceptors’ members with different years of teaching experience do not differ in their perceptions of the effectiveness of clinical instructors’ characteristics, as shown in Figure 3.
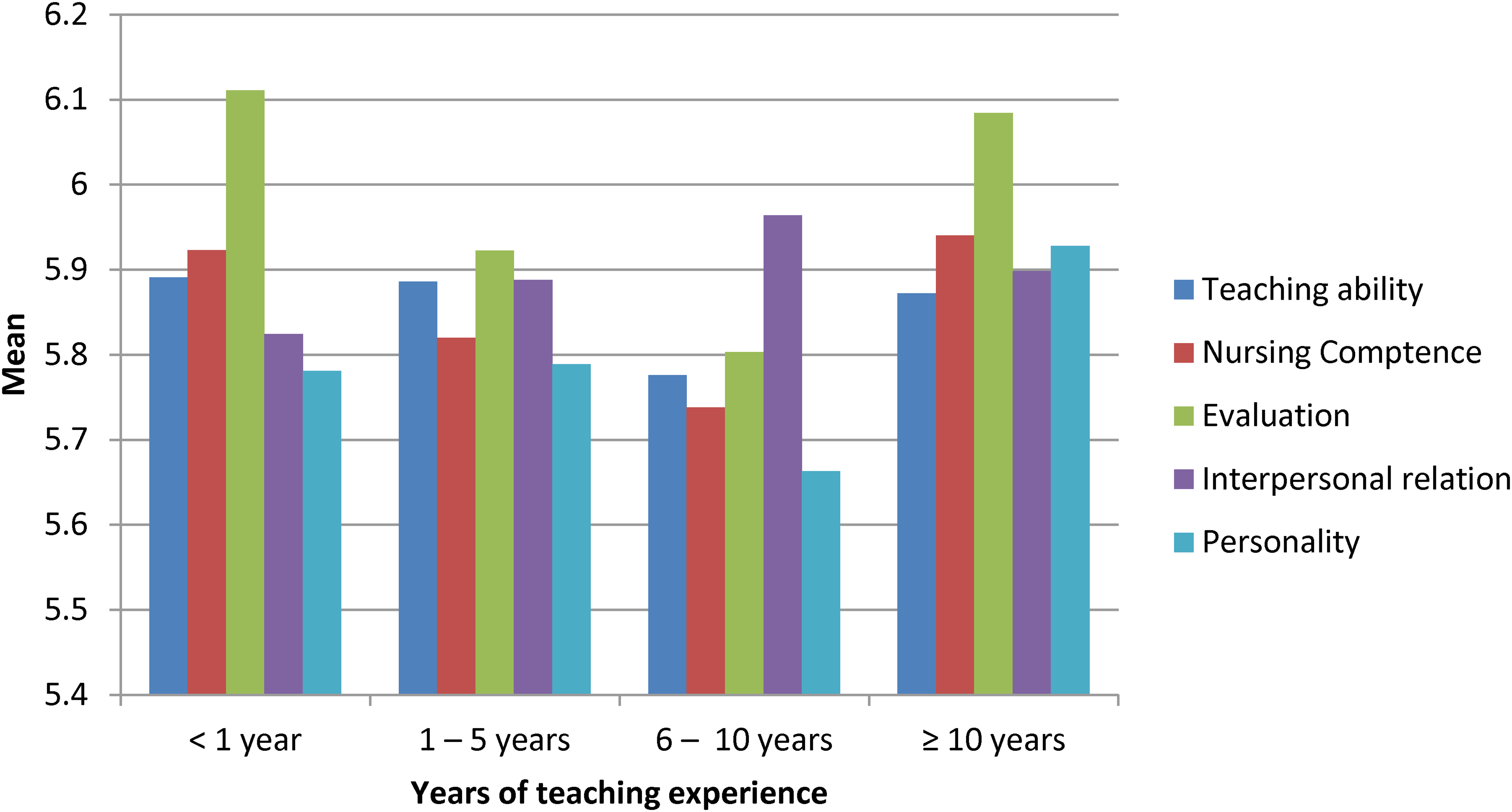
Comparing the mean of all characteristics between preceptors according to their years of teaching experience.
Discussion
The purpose of this study was to identify the characteristics of clinical instructors deemed effective for nursing students, faculty, and preceptors. Overall, all characteristics were considered important by each group, and if we are to be more specific, the characteristic evaluation was considered to be the most important aspect of all participants. Interpersonal skills were the top characteristic among students, while evaluation was among the faculty and preceptors.
Overall, participants perceive evaluation as one of the most effective characteristics of clinical instructors. This refers to the process of evaluating the value or quality of a student's performance or of the products developed by students to represent their learning (Brookhart & Nitko, 2019). Through evaluation, the educator provides answers to the questions, “How well did the student perform?” and “Is the student competent in clinical practice?” In fact, in the medical field, to ensure effective education and patient safety in any learning environment, assessment and evaluation of a student's learning and progress are essential components of the teaching-learning process. This can be done in the classroom, student clinical rotations, skills laboratories, clinical nurse educator roles, staff development programs, preceptorships, or internships. This is implemented by utilizing various but specific assessment and learning measurement tools. This study's findings resonated with numerous studies highlighting evaluation skills as the most important clinical instructors’ attribute at any level of nursing education (Gignac-Caille & Oermann, 2001).
Students Perceptions
As for nursing students, interpersonal skills and teaching ability were perceived as the most important characteristics of a clinical instructor. Interpersonal skills refer to the relationship between clinical preceptors and their students in clinical settings (Koy, 2015). When nursing students encounter problems or are unable to perform a task properly, they should approach their clinical preceptors and establish an environment of mutual respect. According to a previous study, nursing students perceived intrapersonal skills as the first and most important characteristic, which indicates the value of relationships during the learning process (Koy, 2015). As a matter of fact, the main purpose of university-level education is to promote professional socialization and help students who have just begun their nursing education integrate their knowledge, skills, attitudes, values, and ethical standards into their behavior (Altıok & Üstün, 2014). The instructors’ or preceptors’ personalities, teaching abilities, and supportive types of communication facilitate the development of interpersonal relation–friendly interrelationships, promoting the organizational socialization and retention of students or neophyte nurses (Jang & Kim, 2019). Furthermore, teaching ability is the second most important characteristic considered by students. Since students have limited knowledge and clinical experience, they are more dependent on their clinical instructors to demonstrate the skills, attitudes, and values they are developing through clear instruction (Gignac-Caille & Oermann, 2001). Researchers have also found that the best clinical teachers possess a high level of clinical competence, knowledge of effective teaching techniques, and a good level of interpersonal skills. According to students, teaching and learning theory, the curriculum, the clinical setting, and a teacher's understanding of the learner were all important factors influencing their perception of effective clinical teaching. Clinical teachers who provide effective clinical teaching traits will always be valued as good role models (Gignac-Caille & Oermann, 2001).
Faculty Perceptions
A major responsibility of the faculty is to create an environment that encourages students to develop a variety of skills. Therefore, the faculty should match each student with a clinical instructor who has the necessary skills for a profession. Faculty members perceived evaluation as the most important characteristic of the preceptors. In a previous study, faculty reflected on the importance of providing students with appropriate feedback as part of the evaluation process (Gignac-Caille & Oermann, 2001). For faculty, evaluation is important because it reflects the competence of preceptors and students. A high evaluation indicates that an effective training program has been delivered. Furthermore, interpersonal skills are perceived as the second most important characteristic. For faculty, interpersonal skills are important because students are under a lot of stress when they are in clinical practice. Students are anxious about making mistakes and are nervous that patients and their families won't accept them, or that the primary nurse or other members of the team may evaluate or even criticize them. During these circumstances, it is extremely important for the students to have a preceptor who is supportive and friendly (Koy, 2015).
Preceptors Perceptions
Due to their dual roles as teachers and mentors, clinical preceptors perceive evaluation and intrapersonal skills as the most important characteristics. A preceptor, just like faculty members, views evaluation as an essential part of clarifying what positive effects the students have been able to attain as a result of their experiences under their care. If a preceptor has higher evaluations, it is more likely that they are capable of teaching and providing knowledge to students. Furthermore, having interpersonal skills is important for a preceptor because it will allow the students to accept the work environment and staff more readily and give them more opportunities to learn. In a previous study conducted in Cairo, interpersonal skills were perceived as the second most important aspect of effective clinical teaching, which is consistent with our findings (Banan et al., 2017). This enables students to interact and communicate with others more confidently and relaxedly, which can reduce stress in the clinical setting.
However, in our study, nursing competence and personality were perceived by all participants to be the least important characteristics of a clinical instructor. A recent study conducted with nurse trainees in Riyadh has shown that a clinical instructor's personality is one of the most important characteristics, while competence also has a relatively low score (Hababeh & Lalithabai, 2020). It could be possible that some nursing students may perceive personality as the least important characteristic of their clinical instructor due to the emphasis on technical skills, as nursing education is heavily focused on developing clinical skills necessary for patient care. Therefore, students may prioritize the development of clinical skills rather than the instructor's personality. On the other hand, professional competence was ranked as the most important characteristic of a clinical instructor, and personality ranked third in a study among Omani nursing students (Madhavanprabhakaran et al., 2013). The results of this study do not match ours, perhaps because students do not fully understand the crucial role that competence plays in their educational outcomes. Moreover, competence can be perceived as intimidating and authoritarian, which may create a negative perception of instructors who possess these qualities. Students, faculty, and preceptors all agree that clinical teachers’ best characteristics relate to evaluation, interpersonal skills, and teaching abilities. Based on the findings of this study, it can be recommended that clinical instructors use the NCTEI as a self-assessment tool for teacher effectiveness and to provide feedback to them to help them incorporate desirable behaviors into their practice. There is a need to emphasize a clinical instructor's responsibilities and the characteristics of an effective clinical instructor when organizing orientation programs and workshops for new clinical instructors.
Strengths and Limitations
The strength of this study is its intent to compare effective clinical characteristics between students, faculty, and preceptors’ perspectives. The study recruited nursing students, faculty, and preceptors from different programs throughout the kingdom, thus offering high external validity. However, this study has several limitations. The study involved only a one-time measurement, which cannot assess causal relationships. Only Saudi institutions participated in this study, so the results cannot be generalized to all nursing programs worldwide.
Conclusions
Students, faculty, and preceptors all agree that clinical teachers’ best characteristics relate to evaluation, interpersonal skills, and teaching abilities. Based on the findings of this study, it can be recommended that clinical instructors use the NCTEI as a self-assessment tool for teacher effectiveness and to provide feedback to them to help them incorporate desirable behaviors into their practice. There is a need to emphasize a clinical instructor's responsibilities and the characteristics of an effective clinical instructor when organizing orientation programs and workshops for new clinical instructors.
Supplemental Material
sj-docx-1-son-10.1177_23779608241298427 - Supplemental material for Nursing Students, Faculty, and Preceptors Perception of Effective Characteristics of Clinical Instructor: A Cross-Sectional Study
Supplemental material, sj-docx-1-son-10.1177_23779608241298427 for Nursing Students, Faculty, and Preceptors Perception of Effective Characteristics of Clinical Instructor: A Cross-Sectional Study by Shmayil F. Buanz, Abrar Y. Alsenayien, Hanin A. Altharman, Rawan I. Alnaqi, Maria Blesilda B. Llaguno, Ola Mousa and Rayan A. Siraj in SAGE Open Nursing
Supplemental Material
sj-docx-2-son-10.1177_23779608241298427 - Supplemental material for Nursing Students, Faculty, and Preceptors Perception of Effective Characteristics of Clinical Instructor: A Cross-Sectional Study
Supplemental material, sj-docx-2-son-10.1177_23779608241298427 for Nursing Students, Faculty, and Preceptors Perception of Effective Characteristics of Clinical Instructor: A Cross-Sectional Study by Shmayil F. Buanz, Abrar Y. Alsenayien, Hanin A. Altharman, Rawan I. Alnaqi, Maria Blesilda B. Llaguno, Ola Mousa and Rayan A. Siraj in SAGE Open Nursing
Footnotes
Data Availability
Declaration of Conflicting Interests
Ethical Approval
Funding
Informed Consent
Supplemental Material
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
