Abstract
Introduction
Nurses working in critical care units often encounter complex and challenging situations (Jones et al., 2016), witnessing significant human pain and suffering (Sacco et al., 2015). The stresses faced by these nurses contribute to a high incidence of burnout (Beevi et al., 2019). Among the emotional challenges they confront are end-of-life issues, ethical decision-making, and the ongoing suffering of patients, compounded by futile medical interventions, inadequate communication, and numerous demands from patients’ families (Sheikhbardsiri et al., 2022; van Mol et al., 2015). Therefore, the presence of compassion in nurses is essential for enhancing the quality of care (Zamanzadeh et al., 2018). Compassion is a fundamental aspect of clinical nursing (Habib et al., 2023) and patient-centered care (Pehlivan & Güner, 2020). It encompasses empathy and respect for patients’ opinions, values, and beliefs (Babaei & Taleghani, 2019). Thus, nurses must not only possess the requisite knowledge and technical skills for patient care but also embody compassion (Tehranineshat et al., 2019).
Compassionate care involves interactive communication, where nurses strive to understand patients’ concerns by empathizing with their situations and actively addressing these concerns (Babaei & Taleghani, 2022). The essence of compassionate care lies in responding to patients’ physical, spiritual, and emotional needs (Pehlivan & Güner, (2020).
Providing compassionate nursing care not only enhances patient satisfaction and safety but also leads to time and cost savings, increased staff fulfillment, and improved coping skills (Dalvandi et al., 2019). Moreover, greater compassion correlates with better patient outcomes (Roze des Ordons et al., 2019) and is a vital component in delivering high-quality nursing care (Pehlivan & Güner, 2020; Zamanzadeh et al., 2018).
To achieve the highest quality of healthcare, attention to patient safety is crucial (Jabarkhil et al., 2021). Reports indicate that 5 to 10 percent of health-related costs stem from unsafe clinical services that lead to patient harm (Farahani et al., 2021). To enhance patient safety, nurses must prioritize the culture of patient safety. This culture is defined as the acceptance of patient safety as a top priority and a shared value within the organization, continuously seeking to minimize harm resulting from the provision of care (Salamat et al., 2019). A strong safety culture is linked to improved patient health outcomes (Hessels et al., 2019). Evidence shows that a focus on patient safety culture—characterized by transparency in error reporting, using data to improve processes, reducing blame on individuals, fostering teamwork, maintaining clear communication, and encouraging collaboration for the benefit of patients (Taghavi Larijani & Ghane, 2018)—is associated with a reduction in missed nursing care (MNC) (Hessels et al., 2019).
MNC refers to any aspect of patient care that has been completely or partially omitted or delayed (Kalisch & Williams, 2009). Research has shown that the rate of MNC varies between 73.4% and 86% (Ball et al., 2016; Lake et al., 2016). MNC significantly negatively impacts patient outcomes, the quality of nursing care (Recio-Saucedo et al., 2018), and patient safety, and it has been associated with an increased incidence of 30-day mortality (Ball et al., 2018).
Review of Literature
Recent emphasis has been placed on the importance of compassion among healthcare professionals, patients, and families in the healthcare sector (Kim & Lee, 2020). As a result, the International Council of Nurses has identified compassion as one of the five fundamental professional values all nurses should uphold (ICN, 2012).
In Kim's study (2020), it was shown that there is a negative correlation between compassion competency in nurses and missed nursing care. It seems that nurses who embrace compassionate knowledge, skills, and attitudes can respond more sensitively to the diverse needs of patients and may be less likely to omit necessary nursing care (Kim & Lee, 2020).
Although compassionate care by nurses is considered essential for establishing a therapeutic relationship with patients (Alharbi et al., 2020), modern nursing is increasingly based on quantitative evidence and technical skills, with little attention to ethics and compassion. In a study conducted by Faghihi et al. (2024), it was found that mean compassionate care score among nurses caring for elderly patients is high (Faghihi et al., 2024). Meanwhile, the study by Dalvandi et al. (2019) revealed a significant discrepancy from the patients’ perspective between the importance of compassionate care and its delivery by nurses (Dalvandi et al., 2019). Nurses in critical care units have a greater need for compassion in their care due to the specific conditions of patients and their closer relationships with patients and their families compared to nurses in other units (Babaei & Taleghani, 2022). The high workload of nurses working in these units may negatively impact patient safety and the quality of service delivery (Bergman et al., 2021).
Given the importance of compassionate care as a fundamental element in enhancing the quality of healthcare services and its potential impact on patient safety and missed nursing care in critical care units, this research aimed to investigate the relationship between compassionate care, missed nursing care, and patient safety culture from the perspective of nurses working in these settings. If a relationship among these factors is confirmed, optimal conditions can be established to encourage compassionate care among critical care nurses. By implementing such measures, we can reduce missed nursing care and enhance the culture of patient safety.
Methodology
The design of this study is descriptive-analytical.
Selection and Description of Participants
The participants in this study included all nurses working in Intensive Care Units (ICU) and Coronary Care Units (CCU). Inclusion criteria consisted of male and female nurses having a bachelor's degree or higher and a minimum of six months of work experience in critical care units. The exclusion criterion was the submission of incomplete questionnaires.
Data Collection
Data were collected through convenience sampling over a four-month period in 2023 across four hospitals, which had the highest number of nurses working in critical care units. After obtaining permission from the ethical committee, the researchers informed eligible nurses about the research objectives and encouraged them to participate in the study. Written informed consent was obtained from all participants, and all necessary information regarding privacy was provided.
Measurements
In the present study, four questionnaires were used: Demographic Information, Compassionate Care, the MISSCARE Survey, and Patient Safety Culture.
The demographic information questionnaire included questions about age, gender, education, type of unit, work experience, shift type, overtime hours, intention to leave the job, adequacy of staff numbers, the number of patients cared for during each shift, and the number of patients admitted or discharged during the shift.
The Compassionate Care Questionnaire, consisting of 28 items, was designed by Tehrani Neshat et al. (2021) in Iran. This questionnaire encompasses the domains of professional performance, continuous follow-up, patient-centered performance, and empathetic communication. The minimum score is 28 and the maximum score is 140. A high score indicates good compassionate care, while a low score reflects weaknesses in compassionate care. Based on the score range, the lower third (poor) is 28–65, the middle third (average) is 66–103, and the upper third (good) is 104–140. The validity of the questionnaire was evaluated through content validity, while construct validity was assessed using Exploratory Factor Analysis (EFA), Confirmatory Factor Analysis (CFA), and convergent validity.
The reliability of the questionnaire was reported with a Cronbach's alpha coefficient and intraclass consistency of 0.91 and 0.94, respectively (Tehranineshat et al., 2021). In the current study, the reliability of this questionnaire was obtained as 0.94.
The MISSCARE Survey was developed by Kalisch and Williams (2009) and consists of two parts: the level of missed nursing care (24 items) and the reasons for missed nursing care (17 items). In the section measuring the level of missed nursing care, dimensions such as necessary care, secondary care, and supportive care were evaluated using a Likert scale ranging from “always missed” to “never missed.” In the section on reasons for missed nursing care, factors such as labor resources, material resources, communication, responsibility, and unpredictable situations were assessed using a Likert scale from “important reason” to “no reason.” The validity of the MISSCARE Survey was tested using EFA (Kalisch & Williams, 2009).
MISSCARE Survey has a minimum score of 24 and a maximum score of 120. A high score indicates the highest level of missed nursing care, while a low score indicates the lowest level of missed nursing care. In the part of reasons, the minimum score is 17 and the maximum is 68. A high score indicates significant reasons for missed care, while a low score indicates less important reasons for missed nursing care.
In Iran, this survey was psychometrically evaluated by Hosseini et al (2022). The content validity ratio (CVR) and content validity index (CVI) were used to evaluate content validity. Construct validity was assessed using CFA. The internal consistency measured by Cronbach's alpha was 0.933 for the first part and 0.910 for the second part (Hosseini et al., 2022). In this study, the reliability with Cronbach's alpha coefficient was 0.90 for the first part and 0.89 for the second part.
The Patient Safety Culture Questionnaire was designed by the Agency for Healthcare Research and Quality in 2004 and contains 42 items across 12 dimensions (Westat et al., 2018). The items were answered on a five-point Likert scale, from completely disagree (1) to completely agree (5) or from never (1) to always (5).
This questionnaire was psychometrically evaluated in Iran by Moghri and colleagues in 2012. The construct validity of the questionnaire was assessed using CFA. The internal consistency of the questions in the Persian questionnaire ranged from 0.57 to 0.8. The Cronbach's alpha related to the internal consistency of all domains was 0.82, and the Spearman-Brown coefficient was 0.81 (Moghri et al., 2012). In the present study, the Cronbach's alpha coefficient for this questionnaire in all dimensions was 0.75.
For scoring the questionnaire, there were a few negatively worded items in the questionnaire that were reverse coded. If the proportion of respondents who answered “completely agree”/“agree”, or “always”/“most of the time” on each item was more than 50%, this was considered as positive, otherwise (below 50%) as the negative point of the safety culture (Amiri et al., 2018).
Sample Size
The sample size was determined using G*Power software with a power of 90%, α:0.05 (Type I error), and utilizing information from a similar previous study (7) (the relationship between compassionate competence and missed nursing care with r = 0.215). The minimum sample size was set at 223 individuals, and with a 15% dropout rate, it was determined to be 256 individuals. Due to the need for a larger number of samples for higher result validity, 300 questionnaires were distributed among individuals, and ultimately, 290 questionnaires were returned.
The formula for determining sample size is as follows: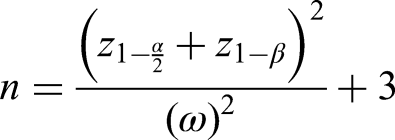
Ethical Considerations
After obtaining permission from the vice-chancellor and the Ethics Committee (IR.SUMS.NUMIMG.REC.1402.035), the researchers explained the study's objectives to eligible nurses. After obtaining written informed consent for participation in the research, they distributed the questionnaires among them and collected them upon completion by the nurses. Confidentiality of information was maintained throughout the data collection process. Also, the permission for using data collection tools was obtained from the tools designers.
Statistical Analysis
All data were analyzed using SPSS software version 24. Descriptive and analytical analyses were employed. The Kolmogorov-Smirnov test was used to examine the normal distribution of the data, indicating a non-normal distribution. For descriptive tests, frequency, percentage, mean, and standard deviation were measured. Categorical variables were examined using the Kruskal-Wallis test. The Spearman correlation coefficient was used to determine the relationship between variables. Statistically, p-value of less than 0.05 was considered significant.
Results
Out of the 300 questionnaires distributed among nurses, 10 were excluded from the study due to incomplete responses. Demographic findings from the 290 study participants revealed that the mean age of nurses was 32.83 ± 5.58 years, average working hours were 49.8 ± 7.79 h per week, work experience averaged 8.33 ± 4.93 years, and experience in the critical care unit was 5.5 ± 4.07 years. Additional characteristics are presented in Table 1.
The Demographic Characteristics of Nurses Working in Critical Care Units.

The overall mean score for compassionate care among nurses was 125.27 ± 12.10. Additionally, the mean score for missed care was 49.19 ± 10.95, with the highest missed care occurring in the domain of supportive care (11.11 ± 3.14). Among the reasons for missed care, human resources scored the highest (11.34 ± 1.29), while the communication domain had the lowest score regarding missed nursing care (11.79 ± 2.96). Table 2 presents the mean and standard deviation of the subdimensions for all three variables: compassionate care, the level of missed care, and the reasons for missed nursing care.
Mean and Standard Deviation of Compassionate Care Scores, Level of Missed Nursing Care, and its Reasons in Nurses Working in Adult Critical Care Units.

This study demonstrated a statistically significant relationship between the score of compassionate care and both gender (P = 0.009) and the type of nursing shifts (P = 0.004). Specifically, women provided more compassionate care to patients than men. Statistical analyses indicated that nurses with rotating shifts had lower scores for compassionate care compared to those with fixed shifts. Furthermore, the Spearman correlation test revealed a direct and significant relationship between work experience and the average score of compassionate care (r = 0.14, p = 0.017), indicating a positive but weak correlation.
Other results of the study indicate a significant relationship between various factors and the average score of missed nursing care. These factors include the type of ward (P = 0.004), working hours (P = 0.001), having overtime (P = 0.001), willingness to leave the job (P = 0.000), the number of patients per shift (P = 0.007), and the number of admitted patients (P = 0.019). Specifically, the average score of missed nursing care was higher among nurses working in coronary care units, those with longer working hours and overtime, and those managing more admitted patients and patients under care during their shifts.
Additionally, the frequency distribution of the average positive and negative responses to the dimensions of the patient safety culture questionnaire is presented in Table 3. This study revealed that the strongest dimension of patient safety culture, from the nurses’ perspective, was organizational learning-continuous improvement (97.6% positive responses), while the weakest was staffing (11.4% positive responses), respectively.
Frequency Distribution of the Average Positive and Negative Responses to the Dimensions of the Patient Safety Culture Among Nurses Working in Adult Critical Care Units.

The Spearman correlation test between compassionate care, missed nursing care, and sub-dimensions of patient safety culture revealed a statistically significant inverse relationship between compassionate care and the level of missed nursing care (r = −0.158, P = 0.007). Additionally, there were direct and significant relationships between compassionate care and the following dimensions of patient safety culture: organizational learning-continuous improvement (r = 0.202, P = 0.001), management support for patient safety (r = 0.163, P = 0.006), feedback and communication about errors (r = 0.249, P = 0.000), communication openness (r = 0.116, P = 0.049), and staffing (r = 0.133, P = 0.024).
The correlation test also showed that there was an inverse and significant correlation between the level of missed nursing care and teamwork within units (r = −0.159, P = 0.007), supervisor/manager expectations & actions promoting patient safety (r = −0.168, P = 0.004), management support for patient safety (r = −0.148, P = 0.012), overall perceptions of patient safety (r = −0.131, P = 0.026), and feedback and communication about errors (r = −0.285, P = 0.000).
Additionally, there was a positive and significant relationship between missed nursing care and staffing (r = 0.184, P = 0.002). The correlation coefficients of compassionate care with the level of missed nursing care and patient safety culture are presented in Table 4.
The Relationship and 95% Confidence Interval Between Compassionate Care, the Level of Missed Nursing Care and Dimensions of Patient Safety Culture among Nurses Working in Adult Critical Care Units.

p value <0.05
p value <0.01
Discussion
This research aimed to examine the relationship between compassionate care, missed nursing care, and patient safety culture from the perspective of nurses working in the critical care units.
The study found that female nurses, those working rotating shifts, and those with more work experience provided more compassionate care to patients. Previous studies have shown that female nurses tend to have a higher mean score of compassionate care compared to their male counterparts (Dalvandi et al., 2019; Siddiqui et al., 2022). This difference may be attributed to the gender and social characteristics of women, which may lead them to be more inclined toward compassionate care (Madsen et al., 2024). Furthermore, as nurses gain more work experience, they acquire additional skills and insights that enable them to better understand patients’ needs, allowing for greater empathy and compassion in care delivery (Alilyyani et al., 2024).
Additionally, other findings from this study indicated a direct relationship between long working hours, overtime, the number of patients per shift, and the number of admitted patients with an increase in level of missed care in critical care units. The stressful environment of critical care, coupled with prolonged working hours, can negatively impact healthcare staff's ability to concentrate, make accurate decisions, and provide appropriate care (Dijkstra et al., 2023). As the number of patients per shift rises, the time allocated to each patient decreases (Dehnoei et al., 2024), leading to increased workload pressure for staff (Han et al., 2024).”
The research results on patient safety culture indicated that the strongest dimension was organizational learning and continuous improvement, which aligns with the findings of studies by Alshammari et al. (2024) and Jabarkhil et al. (2021). Considering the central role of nurses in patient safety, they are given the opportunity to learn from past errors and adverse events through organizational learning (Sarfraz et al., 2023). Furthermore, the weakest dimension of patient safety culture was reported to be staffing. In situations of staff shortages, nurses are compelled to manage a high workload; this may lead to fatigue, burnout, and an increase in medical errors (Albalawi et al., 2020). During periods of high workload, especially in critical care units, patient safety is at greater risk.
The present research indicated a significant inverse relationship between the scores of compassionate care and missed nursing care, which is consistent with the findings of the study by Kim et al. (Kim & Lee, 2020). However, this correlation is somewhat weak, which may be attributed to the sampling method (convenience rather than random sampling).
When nurses face excessive workloads, their ability to provide compassionate care may diminish (Julia et al., 2024). In such situations, nurses may need to focus on performing basic tasks and may pay less attention to the emotional and spiritual needs of patients (Duhalde et al., 2023). Therefore, decreasing the patient-to-nurse ratio in healthcare settings could help nurses provide compassionate care to their patients (Ghafourifard et al., 2022). Iranian nurses often work excessive overtime for minimal pay to address the nursing shortage, leading to fatigue, burnout, and dissatisfaction (Keshavarzi et al., 2024). These factors create an environment that hinders the delivery of quality, safe, and compassionate care (Galehdarifard et al., 2024).
In examining the relationship between average scores of compassionate care and dimensions of patient safety culture, we observed a direct and significant correlation between compassionate care and several dimensions, including organizational learning and continuous improvement, management support for patient safety, feedback and communication about errors, communication openness, and staffing. Research indicates that fostering a culture of compassionate care in healthcare organizations enhances organizational learning and continuous improvement (Abid et al., 2022).
A study by Salminen-Tuomaala and Seppälä (2023) revealed a direct and significant relationship between compassionate care and managerial support for patient safety. Managers can create a supportive work environment and encourage employees to provide compassionate care (Salminen-Tuomaala & Seppälä, 2023). Moreover, providing constructive and supportive feedback regarding errors increases the sense of psychological safety among employees, encouraging them to express their concerns (Øen et al., 2024).
Studies show that individuals who are open and transparent in their communications typically experience a higher level of compassionate care, as open communication helps establish emotional connections and fosters social support (Habib et al., 2023). Compassionate care also helps employees cope better with job challenges and pressures (Flowers et al., 2024), which can lead to reduced turnover and resignation rates, as well as increased staff retention (Habib et al., 2023).
Other findings showed that there is a relationship between the mean score of missed nursing care and some dimensions of safety culture; such that the level of missed nursing care is inversely and significantly related to teamwork within units, supervisor/manager expectations & actions promoting patient safety, management support for patient safety, overall perception of patient safety, feedback and communication about errors. Insufficient collaboration among staff leads to heavy workload (House et al., 2024), which can increase the level of missed care. On the other hand, the lack of attention from managers to patient safety reduces the willingness of staff to take patient safety-promoting actions, leading to an increase in missed nursing care (Chaboyer et al., 2021). The study by Phelan and Kirwan showed that insufficient and untimely feedback from staff regarding errors weakens their perception of communications related to errors, which can lead to increased missed care and reduced organizational efficacy (Phelan & Kirwan, 2020).
The results of the present study indicate a direct and significant relationship between the mean score of missed nursing care and staffing levels. This relationship can be explained by the fact that even with an adequate number of staff, weak teamwork can lead to a greater incidence of missed care (Ghezeljeh et al., 2020). Therefore, considering the importance of addressing missed nursing care to ensure patient safety, it is recommended to study and thoroughly investigate the events leading to errors, identify their root causes, and provide sufficient training.
Strengths and Limitations
While prior studies have assessed patient safety culture and missed nursing care separately, this study is one of the first that assessed the relationship between compassionate care, patient safety culture, and missed nursing care. Although compassionate care is not a new concept in nursing literature, its quantitative measurement is relatively recent, and limited studies have addressed it.
The limited number of hospitals, convenience sampling and focus on nurses in adult critical care units make generalization difficult. The self-reporting nature of the questionnaires and exaggeration in responses can negatively impact the results.
Implications for Nursing Practice
Given the significant inverse relationship between compassionate care and missed nursing care, as well as the positive and significant relationship between compassionate care and patient safety culture in critical care units, nursing managers and hospital officials can improve the work environment for nurses and enhance the quality of nursing care by implementing training programs.
Greater emphasis on compassionate care in nursing education and the integration of moral and human virtues in care can help to improve the quality of nursing services. Nursing managers can play a crucial role by identifying and addressing barriers to compassionate care. Reducing nurses’ workloads, increasing organizational support, and fostering an environment conducive to delivering compassionate care can minimize missed nursing care and thereby enhance patient safety. It is suggested that future studies evaluate the impact of compassionate care promoting programs on the rate of missed nursing care, patient safety culture, and other patient safety outcomes among nurses in critical care units or those working in general units.
Conclusion
This study demonstrated that compassionate care is significantly related to various dimensions of patient safety culture and the level of missed nursing care. It also showed that compassionate care is associated with a lower level of missed nursing care.
